Accessibilité
Afin d'être accessible au plus grand nombre, nous vous informons que vous avez la possibilité de modifier la taille d’affichage du contenu de notre site. Pour cela, voici les commandes à reproduire à l'aide de votre clavier :

Numéros d'urgence

- Standard et urgences

Présentation de l’équipe de Neuro-Radiologie Interventionnelle
L'équipe médicale NRI
Unité de Neuroradiologie Interventionnelle

Dr Richard BIBI
Responsable d’unité

Pr Denis HERBRETEAU
Professeur des Universités Praticien Hospitalier

Dr Grégoire BOULOUIS
Praticien Hospitalier

Dr Héloïse IFERGAN
Praticien Hospitalier

Dr Kevin JANOT

Dr Fouzi BALA
Service de Radiologie, Neuroradiologie Diagnostique Interventionnelle
Docteur Baptiste MOREL
Chef de Service
Pr Laurent BRUNEREAU
Chef de Pôle Imagerie
L’équipe est composée par ailleurs de :
- 14 manipulateurs d’électroradiologie médicale,
- 5 secrétaires dédiées,
- 2 attachés de recherche clinique.
Contact et prise de rendez-vous
Aller au contenu | Navigation | Accès directs | Connexion
- Bibliothèques
- Orientation & Insertion
- Nos unités de recherche
- Nos marchés publics
- Faculté Arts & Sciences Humaines (ASH) Voir le site
- Faculté Centre d'Études Supérieures de la Renaissance Voir le site
- Faculté Droit Economie & Sciences Sociales Voir le site
- Faculté IAE Voir le site
- IUT IUT de Blois Voir le site
- IUT IUT de Tours Voir le site
- Faculté Lettres & Langues Voir le site
- Faculté Médecine Voir le site
- Faculté Odontologie Voir le site
- Faculté Pharmacie Voir le site
- Ecole Polytech Tours Voir le site
- Faculté Sciences & Techniques Voir le site
- GIS Collegium Santé Voir le site
Personnel hébergé
M. Laurent Brunereau
Coordonnées.
Avenue de la République 37170 CHAMBRAY LES TOURS
Discipline(s)
Cardiovascular magnetic resonance in heart transplant patients: diagnostic value of quantitative tissue markers: T2 mapping and extracellular volume fraction, for acute rejection diagnosis
Affiliations.
- 1 Department of Cardiothoracic Surgery, University François Rabelais, Tours, France. [email protected].
- 2 Department of Radiology, University François Rabelais, Tours, France. [email protected].
- 3 Department of Cardiothoracic Surgery, University François Rabelais, Tours, France.
- 4 Department of Radiology, University François Rabelais, Tours, France.
- 5 Department of Anatomopathology, University François Rabelais, Tours, France.
- PMID: 30153847
- PMCID: PMC6114788
- DOI: 10.1186/s12968-018-0480-9
Background: The diagnosis of acute rejection in cardiac transplant recipients requires invasive technique with endomyocardial biopsy (EMB) which has risks and limitations. Cardiovascular magnetic resonance imaging (CMR) with T2 and T1 mapping is a promising technique for characterizing myocardial tissue. The purpose of the study was to evaluate T2, T1 and extracellular volume fraction (ECV) quantification as novel tissue markers to diagnose acute rejection.
Methods: CMR was prospectively performed in 20 heart transplant patients providing 31 comparisons EMB-CMR. CMR was performed close to EMB. Images were acquired on a 1.5 Tesla scanner including T2 mapping (T2 prepared balanced steady state free precession) and T1 mapping (modified Look-Locker inversion recovery sequences: MOLLI) at basal, mid and apical level in short axis view. Global and segmental T2 and T1 values were measured before and 15 min (for T1 mapping) after contrast administration.
Results: Acute rejection was diagnosed in seven patients: six cellular rejections (4 grade IR, 2 grade 2R) and one antibody mediated rejection. Patients with acute rejection had significantly higher global T2 values at 3 levels: 58.5 ms [55.0-60.3] vs 51.3 ms [49.5-55.2] (p = 0.007) at basal; 55.7 ms [54.0-59.7] vs 51.8 ms [50.1-53.6] (p = 0.002) at median and 58.2 ms [54.0-63.7] vs 53.6 ms [50.8-57.4] (p = 0.026) at apical level. The area under the curve (AUC) for each level was 0.83, 0.79 and 0.78 respectively. Patients with acute rejection had significantly higher ECV at basal level: 34.2% [32.8-37.4] vs 27.4% [24.6-30.6] (p = 0.006). The AUC for basal level was 0.84. The sensitivity, specificity and diagnosis accuracy for basal T2 (cut off: 57.7 ms) were 71, 96 and 90% respectively; and for basal ECV: (cut off 32%) were 86, 85 and 85% respectively. Combining basal T2 and basal ECV allowed diagnosing all acute rejection and avoiding 63% of EMB.
Conclusions: In heart transplant patients, a combined CMR approach using T2 mapping and ECV quantification provides a high diagnostic accuracy for acute rejection diagnosis and could potentially decrease the number of routine EMB.
Keywords: Acute cardiac rejection; Cardiovascular magnetic resonance; Endomyocardial biopsy; T1 and T2 mapping.
- Acute Disease
- Case-Control Studies
- Graft Rejection / diagnostic imaging*
- Graft Rejection / immunology
- Graft Rejection / pathology
- Heart Transplantation / adverse effects*
- Magnetic Resonance Imaging*
- Middle Aged
- Myocardium / pathology*
- Predictive Value of Tests
- Prospective Studies
- Reproducibility of Results
- Risk Factors
- Treatment Outcome
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Pathog Glob Health
- v.108(1); 2014 Jan
Unusual multiple large abscesses of the liver: interest of the radiological features and the real-time PCR to distinguish between bacterial and amebic etiologies
Guillaume desoubeaux.
1 CHU de Tours, Service de Parasitologie – Mycologie – Médecine tropicale, Tours, France
2 Université François Rabelais, CEPR – INSERM U1100 / E.A. 6305, Faculté de Médecine, Tours, France
Hélène Chaussade
3 CHU de Tours, Service de Médecine Interne et Maladies Infectieuses, Tours, France
Marc Thellier
4 CHU La Pitié-Salpêtrière, Laboratoire de Parasitologie – Mycologie, Paris, France
5 Université Pierre et Marie Curie, INSERM U511 / UMR S945 Paris VI, France
6 INSERM U511 / UMR-S 945, Paris, France
Sophie Poussing
Frédéric bastides, eric bailly, philippe lanotte.
7 CHU de Tours, Laboratoire de Bactériologie, Tours, France
8 Université François Rabelais, E5 “Bactéries et risque materno-foetal”, UMR 1282 ISP, INRA, Nouzilly, France
Daniel Alison
9 CHU de Tours, Service de Radiologie Adulte, Tours, France
Laurent Brunereau
Louis bernard, jacques chandenier.
We report a rare case of amebiasis generating 19 large liver abscesses. Such a quantity of abscesses is rare, especially when occurring in a young casual traveler without any immunodeficiency disorders. A possible co-infection was excluded. By contrast, the amebic etiology was confirmed by means of serology and real-time PCR.
Case Report
We report the case of a 36-year-old Caucasian man with febrile diarrhea who presented with a loss of appetite and a severe asthenia. His past medical history was insignificant, and he was up to date with his vaccines. As military personnel in the French army, he had frequently traveled to the French West Indies, French Polynesia, and Senegal during the last 10 years. In the month preceding his hospitalization, he went on a trip to Dakar, Senegal, and then to Martinique in the French West Indies. During these trips he did not take his anti-malarial medical treatment correctly (chemoprophylaxis atovaquone–proguanil). He presented with a fever of 38–40°C, chills, sweats, and myalgia, which were not relieved by taking paracetamol, 4 days after his return to mainland France. The lab report excluded malaria. Parasitological examination of stools and bacterial coprocultures remained negative.
Despite the empirical use of antibiotics (amoxicillin–clavulanic acid), the patient’s symptoms became more severe with hepatomegaly and tender abdomen, particularly in the right upper quadrant. A biological inflammatory syndrome (neutrophil granulocytes = 14.38 g/l; CRP = 419 mg/l) and a hepatic cytolysis with moderate cholestasis were noticed (AST = 91 UI/l; ALT = 44 UI/l; ALP = 108 UI/l; gamma-GT = 66 UI/l). Ceftriaxone was thereafter added to his treatment. The ultrasound scan showed multiple liver hypoechoic lesions with echoic walls, and a hypertrophy of the right liver (length×depth = 20×12 cm) ( Fig. 1 ). An abdominal computed tomography (CT) confirmed the presence of several large hypodense rounded masses ( Fig. 2 ). The inside aspect of the masses seemed to be made up of a heterogeneous liquid, and their edges were irregular. The presence of at least 19 abscesses was observed. The largest lesion measured 96 mm and was located between the V and VI hepatic segments. The smallest one was 40 mm wide. There was no contrast enhancement after injection of intravenous contrast agent. Pan colitis and radiological cholestasis were also observed.

Abdominal ultrasonography showing multiple rounded hypoechoic lesions.

Abdominal-computed tomography (CT) portal-phase showing large hypodense abscesses in all the hepatic segments (helical acquisition; dose length product = 3494 mGy/cm; IV injection of 140 ml iohexol, Omnipaque 350 ® ). The 19 abscesses are individually labeled by large arrows. Edges were irregular, and the content appeared fluid and heterogeneous.
The serology targeting amebiasis was positive: hemagglutination positive at 1∶1280 dilution (IHA Amœbiasis™, Fumouze Diagnostics, Levallois-Perret, France), and indirect immunofluorescence at 1∶800 (Amœba-Spot IF™, BioMérieux, Craponne, France). Concomitantly, all the blood cultures remained sterile. Thereby, an anti-amebic therapy was initiated, based on metronidazole administration at 500 mg tid for 21 days, followed by a luminal amebicide (tiliquinol/tilbroquinol). Within 48 hours the patient had no more fever and his diarrhea had nearly stopped. Neutrophil granulocytes and CRP rate decreased in less than 1 week, to 9.33 g/l and 54 mg/l respectively.
As the patient was still complaining of persistent abdominal pains, a puncture of the painful abscess under the hepatic capsule was performed under CT-guidance ( Fig. 3 ). Standard cultures and the pan-bacterial real-time PCR, targeting the 16S rDNA which were performed directly on the aspirated liquid were all negative. In contrast, the PCR specific for Entamoeba histolytica (16S-like SSU rDNA) was positive ( C t = 27 cycles; standard deviation = 0.104). Briefly, the DNA was extracted using QIAmp DNA mini kit® spin columns (Qiagen™, Courtaboeuf, France). The method performed for amplification and detection was a real-time PCR using a TaqMan 7500® Fast Real-Time PCR System (Applied Biosystems™, Saint Aubin, France). The amplification reactions were performed using 5 μl of a DNA sample in a volume of 20 μl of a mixture that contained a TaqMan Fast Universal PCR Master Mix® (2×) (Applied Biosystems), internal positive control (Applied Biosystems), and the primers for E. histolytica : Eh-196F (5′-AAA TGG CCA ATT CAT TCA ATG A-3′) and Eh-294R (5′-CAT TGG TTA CTT GTT AAA CAC TGT GTG-3′), and the probe Eh-245 (6FAM)-AGG ATG CCA CGA CAA-(NFQ). The thermal cycling conditions were chosen according to TaqMan® Fast protocol (Applied Biosystems) and it consisted of 20 seconds at 95°C followed by 50 cycles of 3 seconds at 95°C, and 30 seconds at 60°C. The detection and the data analysis were performed with TaqMan Fast 7500 software (Applied Biosystems) version 1.4.0.

Computed tomography (CT)-guided aspiration of one of the more accessible abscess showing a sterile brown-purulent liquid. The punctured abscess was located under the capsule in the hepatic segment VI, and initially measured 78×54×80 mm. (A) The aspiration was performed laterally by the means of a trocar (large yellow arrow <$>\vskip-1\scale 80%\raster="rg1"\<$>). (B) The color of the 250 ml harvested fluid appeared macroscopically similar to milk chocolate. (C) The light microscopic observation showed only purulent material with a few degranulated leukocytes (→) and some altered red blood cells (→), but no viable Entamoeba histolytica trophozoites (magnification ×400).
The 6-month follow-up was satisfactory. Neither clinical relapse nor subsequent biological perturbations were noticed. There was a substantial decrease in the size of the liver abscesses. However, the number of lesions persisted.
Amebiasis is a tropical food- and water-borne parasitosis due to the human-specific protozoan E. histolytica. 1 Its worldwide prevalence is estimated at 500 million infected individuals, especially those living in developing countries with low socio-economic level and poor hygienic status. 1 , 2 Potential complications are caused by the trophozoite stage that generates ulceration of the colon and leads to bowel perforations. This first step of invasion could be followed by the hematogeneous dissemination of trophozoites toward organs where abscesses are constituted. Thus, liver abscesses are by far the most common extra-intestinal manifestation of invasive amebiasis. 3 , 4
Although hepatic ultrasound scan is widely used, 5 an abdominal-CT enables a better result allowing more than a 95% detection rate of smaller abscesses and any other associated complications. 6 Amebic abscesses are usually single and are normally located in the right hepatic lobe. 1 , 7 Multiples lesions sometimes occur, but they are infrequently reported. By contrast, a great number of liver abscesses are commonly associated with bacterial etiologies. In 2004, 577 medical records were retrospectively reviewed in order to identify features distinguishing amebic liver abscesses from pyogenic ones. 8 Multivariate analysis found that multiple abscesses are more likely to be associated with pyogenic origin (adjusted odds ratio = 5.34 [2.86–9.96], P < 0.001). Owing to the very unusual tomodensitometric presentation exhibiting 19 large abscesses, the initial hypothesis of a bacterial co-infection was thereafter obviously raised for our patient. Nevertheless, the bio-clinical investigations did not provide evidence of any bacterial involvement: no germs were isolated, 9 and the initial use of antibiotics (i.e. amoxicillin–clavulanic acid, then ceftriaxone) had no effect on the fever or the pain. To our knowledge, such a number of large lesions as a result of an amebic infection have rarely been reported, especially in the case of a young short trip traveler. An interesting reported case referred to 25 amebic liver abscesses in a Belgian woman. 10 However, as she used to live permanently in an endemic area of amebiasis, she was thereby continuously exposed to iterative infections. Excepting this isolated case, observations of multiple amebic liver abscesses have globally remained rare in all the cohorts, and were then limited to a maximum of five or six abscesses, whereas the solitary abscesses represented 65–90% of all these cases. 7 , 11 – 18 Besides, in all these studies, multiples abscesses preferentially occurred in concomitant immunocompromised patients, e.g. HIV-infection, 19 , 20 or in cases of advanced amebiasis, e.g. in subjects exposed to recurrent amebic infections. 3 In our situation, the patient wasn’t known to be immunocompromised, and had only short stays in highly endemic areas of amebiasis.
The present case demonstrates that percutaneous puncture–aspiration enabled the disruption of pain, which was mainly due to abdominal tension induced by the numerous large abscesses. Furthermore, the percutaneous drainage had also a diagnostic role, since the real-time PCR done on the liquid was important in confirming that this was a case of active invasive amebiasis.
According to some authors, image-guided needle aspiration has an evacuation role, and should be considered when there is no clinical improvement after 3 days of taking metronidazole. 21 – 23 It is interesting to note that residual abscesses may persist in 5–28% of cases and remain so for up to 13 years, and this in spite of taking an effective treatment. 24 , 25 In such situations, there is neither fever nor abdominal pain nor jaundice. 4 , 26
Exceptionally numerous large abscesses could be seen during hepatic amebiasis. Faced with such an unusual abdominal-CT scan findings, the use of amebic serology may be of great interest. Furthermore, the real-time PCR test is now considered a smart diagnostic tool. In complicated amebiasis, the percutaneous puncture–aspiration should be considered as an interesting complement to conventional anti-amebic chemotherapy.
Written informed consent was obtained from the patient for publication of this report and any accompanying images.
Financial Support
All authors declare no ongoing financial support. Authors did not receive any funding for the study.
Data have been collected as part of the routine work of University Hospital of Tours.
Transparency Declarations and Conflict of Interest
All authors declare no financial conflict of interest. No funder has played any decision-making role in the research.
All authors have brought their substantial contributions to research design, or the acquisition, analysis, or interpretation of data. They all have been involved in drafting the paper or revising it critically. All authors declare to have given their agreement for the final submission. They confirm that the manuscript is not under editorial consideration in another journal.
The editors have our permission to reproduce any content of the article, after potential acceptation.
Acknowledgments
The authors would like to thank Dr Oussama Mouri (Pitié-Salpêtrière, Paris – France) for his precious help in the implementation of the Entameba dispar/histolytica PCR. The authors are very grateful to Donam Kim, Jérôme Desoubeaux, and Kay Mc Carthy-Cerf from the Pedagogical Department of English learning in the Medical School of Tours University for their precious help with the English translation.
Liver shear wave elastography and attenuation imaging coefficient measures: prospective evaluation in healthy children
- Hepatobiliary
- Published: 08 June 2021
- Volume 46 , pages 4629–4636, ( 2021 )
Cite this article

- Romain Cailloce 1 ,
- Elsa Tavernier 2 ,
- Laurent Brunereau 3 ,
- Adèle Fievet 1 ,
- Céline Falip 1 ,
- Fanny Dujardin 4 ,
- Stéphanie Willot 5 ,
- Frédéric Patat 2 , 3 &
- Baptiste Morel ORCID: orcid.org/0000-0003-4747-3393 1 , 6
631 Accesses
7 Citations
Explore all metrics
Ultrasonographic quantitative measurements enable characterizing the stiffness and viscosity of liver parenchyma. Normal Shear Wave Elastography (SWE) values have been reported in adults and children. The Attenuation Imaging (ATI) coefficient is a measure of local sound energy loss thought to reflect steatosis in adults. The aim of our study was to provide normal SWE and ATI liver values in healthy children.
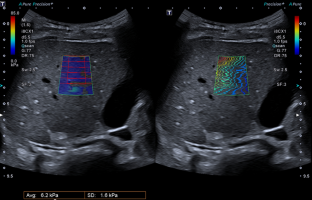
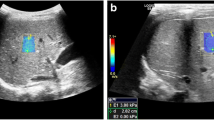
A prospective monocentric study was conducted recruiting 86 children (45 boys and 41 girls) from a single University Hospital between January 2019 and June 2020, having a clinically indicated ultrasound examination, without a known or documented history of liver disease. Examinations were performed using an Aplio i800 (Canon Medical Systems) ultrasound system with an i8CX1 transducer. SWE measurements were obtained using a color map showing an automated measurement area grid overlay. ATI coefficients were generated automatically for each region of interest in the right liver.
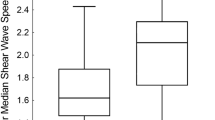
Overall median age for the pediatric population was 106 months (1–180 months; SD 49 months). Children were normal weighted. Liver SWE was available for all children. The median liver SWE was 4.6 kPa [3.3–6.6]. ATI yielded valid measurements in 77 patients. The median ATI coefficient was 0.65 [0.5–0.81] dB/cm/MHz. No impact of age, sex, weight and Body Mass Index was observed.
SWE and ATI liver values were provided in healthy children. The normative quantitative data might be useful to characterize liver parenchyma in children better.
This is a preview of subscription content, log in via an institution to check access.
Access this article
Price excludes VAT (USA) Tax calculation will be finalised during checkout.
Instant access to the full article PDF.
Rent this article via DeepDyve
Institutional subscriptions
Similar content being viewed by others
Reference values of normal liver stiffness in healthy children by two methods: 2D shear wave and transient elastography
Performance of two--dimensional ultrasound shear wave elastography: reference values of normal liver stiffness in children

Two-dimensional ultrasound shear wave elastography for identifying and staging liver fibrosis in pediatric patients with known or suspected liver disease: a clinical effectiveness study
Abbreviations.
Attenuation imaging coefficient
Shear wave dispersion
- Shear wave elastography
Barr RG, Ferraioli G, Palmeri ML, et al (2015) Elastography Assessment of Liver Fibrosis: Society of Radiologists in Ultrasound Consensus Conference Statement. Radiology 276:845–861
DiPaola FW, Schumacher KR, Goldberg CS, Friedland-Little J, Parameswaran A, Dillman JR (2017) Effect of Fontan operation on liver stiffness in children with single ventricle physiology. Eur Radiol 27:2434–2442
Hanquinet S, Rougemont A-L, Courvoisier D, Rubbia-Brandt L, McLin V, Tempia M, Anooshiravani M (2013) Acoustic radiation force impulse (ARFI) elastography for the noninvasive diagnosis of liver fibrosis in children. Pediatr Radiol 43:545–551
Ozturk A, Mohammadi R, Pierce TT, et al (2020) Diagnostic Accuracy of Shear Wave Elastography as a Non-invasive Biomarker of High-Risk Non-alcoholic Steatohepatitis in Patients with Non-alcoholic Fatty Liver Disease. Ultrasound Med Biol 46:972–980
Palmeri ML, Wang MH, Rouze NC, Abdelmalek MF, Guy CD, Moser B, Diehl AM, Nightingale KR (2011) Noninvasive evaluation of hepatic fibrosis using acoustic radiation force-based shear stiffness in patients with nonalcoholic fatty liver disease. J Hepatol 55:666–672
Samir AE, Dhyani M, Vij A, Bhan AK, Halpern EF, Méndez-Navarro J, Corey KE, Chung RT (2015) Shear-wave elastography for the estimation of liver fibrosis in chronic liver disease: determining accuracy and ideal site for measurement. Radiology 274:888–896
Palmeri ML, Wang MH, Dahl JJ, Frinkley KD, Nightingale KR (2008) Quantifying hepatic shear modulus in vivo using acoustic radiation force. Ultrasound Med Biol 34:546–558
Boursier J, Isselin G, Fouchard-Hubert I, Oberti F, Dib N, Lebigot J, Bertrais S, Gallois Y, Calès P, Aubé C (2010) Acoustic radiation force impulse: a new ultrasonographic technology for the widespread noninvasive diagnosis of liver fibrosis. Eur J Gastroenterol Hepatol 22:1074–1084
Bavu E, Gennisson J-L, Couade M, et al (2011) Noninvasive in vivo liver fibrosis evaluation using supersonic shear imaging: a clinical study on 113 hepatitis C virus patients. Ultrasound Med Biol 37:1361–1373
Jung C, Groth M, Petersen KU, Hammel A, Brinkert F, Grabhorn E, Weidemann SA, Busch J, Adam G, Herrmann J (2017) Hepatic shear wave elastography in children under free-breathing and breath-hold conditions. Eur Radiol 27:5337–5343
Bae JS, Lee DH, Lee JY, Kim H, Yu SJ, Lee J-H, Cho EJ, Lee YB, Han JK, Choi BI (2019) Assessment of hepatic steatosis by using attenuation imaging: a quantitative, easy-to-perform ultrasound technique. Eur Radiol 29:6499–6507
Chan W-K, Nik Mustapha NR, Mahadeva S (2014) Controlled attenuation parameter for the detection and quantification of hepatic steatosis in nonalcoholic fatty liver disease. J Gastroenterol Hepatol 29:1470–1476
Dioguardi Burgio M, Ronot M, Reizine E, Rautou P-E, Castera L, Paradis V, Garteiser P, Van Beers B, Vilgrain V (2020) Quantification of hepatic steatosis with ultrasound: promising role of attenuation imaging coefficient in a biopsy-proven cohort. Eur Radiol 30:2293–2301
Paige JS, Bernstein GS, Heba E, et al (2017) A Pilot Comparative Study of Quantitative Ultrasound, Conventional Ultrasound, and MRI for Predicting Histology-Determined Steatosis Grade in Adult Nonalcoholic Fatty Liver Disease. AJR Am J Roentgenol 208:W168–W177
Sugimoto K, Moriyasu F, Oshiro H, Takeuchi H, Abe M, Yoshimasu Y, Kasai Y, Sakamaki K, Hara T, Itoi T (2020) The Role of Multiparametric US of the Liver for the Evaluation of Nonalcoholic Steatohepatitis. Radiology 192665
Trout AT, Xanthakos SA, Bennett PS, Dillman JR (2020) Liver Shear Wave Speed and Other Quantitative Ultrasound Measures of Liver Parenchyma: Prospective Evaluation in Healthy Children and Adults. AJR Am J Roentgenol 214:557–565
Franchi-Abella S, Corno L, Gonzales E, Antoni G, Fabre M, Ducot B, Pariente D, Gennisson J-L, Tanter M, Corréas J-M (2016) Feasibility and Diagnostic Accuracy of Supersonic Shear-Wave Elastography for the Assessment of Liver Stiffness and Liver Fibrosis in Children: A Pilot Study of 96 Patients. Radiology 278:554–562
Matos H, Trindade A, Noruegas MJ (2014) Acoustic radiation force impulse imaging in paediatric patients: normal liver values. J Pediatr Gastroenterol Nutr 59:684–688
Team RC (2015) R: A language and environment for statistical computing. Vienna, Austria; 2014. URL Httpwww R-Proj. Org
Engelmann G, Gebhardt C, Wenning D, Wühl E, Hoffmann GF, Selmi B, Grulich-Henn J, Schenk JP, Teufel U (2012) Feasibility study and control values of transient elastography in healthy children. Eur J Pediatr 171:353–360
Myers RP, Pomier-Layrargues G, Kirsch R, Pollett A, Duarte-Rojo A, Wong D, Beaton M, Levstik M, Crotty P, Elkashab M (2012) Feasibility and diagnostic performance of the FibroScan XL probe for liver stiffness measurement in overweight and obese patients. Hepatol Baltim Md 55:199–208
Gilligan LA, Trout AT, Bennett P, Dillman JR (2020) Repeatability and Agreement of Shear Wave Speed Measurements in Phantoms and Human Livers Across 6 Ultrasound 2-Dimensional Shear Wave Elastography Systems. Invest Radiol 55:191–199
Palabiyik FB, Inci E, Turkay R, Bas D (2017) Evaluation of Liver, Kidney, and Spleen Elasticity in Healthy Newborns and Infants Using Shear Wave Elastography. J Ultrasound Med Off J Am Inst Ultrasound Med 36:2039–2045
Cotoi CG, Quaglia A (2016) Normal liver anatomy and introduction to liver histology. In: Textb. Pediatr. Gastroenterol. Hepatol. Nutr. Springer, pp 609–612
Jeffus S (2014) Histology for Pathologists, 4th Edition. Am. J. Surg. Pathol. 38:
Berzigotti A, De Gottardi A, Vukotic R, Siramolpiwat S, Abraldes JG, García-Pagan JC, Bosch J (2013) Effect of meal ingestion on liver stiffness in patients with cirrhosis and portal hypertension. PloS One 8:e58742
Download references
Acknowledgements
The authors thank the pediatric patients and their parents who agreed to contribute to the study. The authors acknowledge Mr Jean Laurent Lasquellec for his invaluable technical support and Mr John Sheath for his English language assistance. Thanks to Marie Moinier, Madeleine and Capucine. Thanks to Linda Dainese.
No funding was secured for this study. The authors have no financial relationships relevant to this article to disclose.
Author information
Authors and affiliations.
Pediatric Radiology Department, Clocheville Hospital, CHRU de Tours, 49 Boulevard Beranger, 37000, Tours, France
Romain Cailloce, Adèle Fievet, Céline Falip & Baptiste Morel
Clinical Investigation Center, INSERM 1415, CHRU Tours, Tours, France
Elsa Tavernier & Frédéric Patat
Radiology Department, CHRU de Tours, Tours, France
Laurent Brunereau & Frédéric Patat
Pathology, Tours University Hospital, University of Tours, Tours, France
Fanny Dujardin
Pediatric Department, Clocheville Hospital, CHRU de Tours, Tours, France
Stéphanie Willot
UMR 1253, iBrain, Inserm, Université de Tours, Tours, France
Baptiste Morel
You can also search for this author in PubMed Google Scholar
Corresponding author
Correspondence to Baptiste Morel .
Ethics declarations
Conflict of interest.
The authors have no conflict of interest to disclose.
Ethical approval
We declare that all human and animal studies have been approved by the local institutional review board and have therefore been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. We declare that all patients gave informed consent prior to inclusion in this study. We obtained approval by the local Ethics Committee in Human research (RNI- 2020_075).
Informed consent
We declare that all patients gave informed consent prior to inclusion in this study.
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Reprints and permissions
About this article
Cailloce, R., Tavernier, E., Brunereau, L. et al. Liver shear wave elastography and attenuation imaging coefficient measures: prospective evaluation in healthy children. Abdom Radiol 46 , 4629–4636 (2021). https://doi.org/10.1007/s00261-021-02960-w
Download citation
Received : 20 November 2020
Revised : 12 January 2021
Accepted : 15 January 2021
Published : 08 June 2021
Issue Date : October 2021
DOI : https://doi.org/10.1007/s00261-021-02960-w
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Attenuation imaging
- Liver diseases
- Find a journal
- Publish with us
- Track your research
- Se déplacer
- Faits divers
- International
- People & Culture
- L’info en vrai
- Charles Matin
- Apolline Matin
- Face à Face
- Les Grandes Gueules
- Estelle Midi
- Super Moscato Show
- Rothen S'enflamme
- La matinale week-end
- Bons d'achat
- Nous contacter
- BFM Business
- RMC Découverte
- BFM Régions
- Association RMC/BFM
Laurent Alexandre face aux GG - 25/04
Sur le même sujet.

Dr Laurent Alexandre explique l’obsession des milliardaires avec l'IA et la mort

Laurent Alexandre: "Nous sommes actuellement dans une période déterminante de l'IA et il faut que les politiques en prennent conscience"

Le Dr Laurent Alexandre explique la future évolution de l'IA

Taxe touristique : Julie Martinez est mitigée face à cette mesure

"Il y a une systématisation de ce genre de comportement" accuse Bernard de la Villardière

Julie Martinez a été "blessée" par un reportage de Bernard de la Villardière

Bernard de La Villardière traité d'"'islamophobe" et de "raciste", à son retour de tournage, à l'aéroport de Roissy Charles de Gaulle

Famille expulsée d'un HLM : "Tu dois réfléchir aux conséquences !" déplore Alain Marschall

Pour Zohra Bitan : "Ce n'est pas de l'autorité qu'il faut, c'est épauler les profs !"

Prof frappé par un élève : Pour Didier Giraud il faut mettre en place plusieurs points

"Mathilde Panot argumente ses propos par des mensonges !" déclare Zohra Bitan

"Mathilde Panot n'a rien a faire dans un commissariat !" déclare Olivier Truchot

Paris: Elina Dumont dénonce "un nettoyage social" avant les JO

IMAGES
VIDEO
COMMENTS
Service de Radiologie, Neuroradiologie Diagnostique Interventionnelle. Docteur Baptiste MOREL. Chef de Service. Pr Laurent BRUNEREAU. Chef de Pôle Imagerie. L'équipe est composée par ailleurs de : 14 manipulateurs d'électroradiologie médicale, 5 secrétaires dédiées, 2 attachés de recherche clinique.
Laurent BRUNEREAU, Head of Department | Cited by 2,673 | of Centre Hospitalier Universitaire de Tours, Tours | Read 127 publications | Contact Laurent BRUNEREAU
Coordonnées. Avenue de la République 37170 CHAMBRAY LES TOURS. Mail. [email protected].
Laurent Brunereau's 5 research works with 26 citations and 285 reads, including: French survey of sedation practices for pediatric magnetic resonance and computed tomography imaging
Laurent Brunereau MD. Radiology Department, CHU de Tours, Tours, France. Search for more papers by this author. Florence Cavé-Riant MD, Florence Cavé-Riant MD. Cryogenetics Laboratory, Hôpital Lariboisière, Assistance Publique-Hôpitaux de Paris.
Jean-Philippe Cottier, a Anne Pasco, a Sophie Gallas, a Jean Gabrillargues, a Christophe Cognard, a Jacques Drouineau, a Laurent Brunereau, a and Denis Herbreteau a Author information Article notes ... 1 Address reprint requests to J. P. Cottier, MD, Service de Neuroradiologie, CHU Bretonneau, 2 Bd Tonnelé, 37044 Tours, Cédex, France ...
Laurent Brunereau. All authors: Department of Radiology, CHU Bretonneau, 37044 Tours, France. View all articles by this author. Catherine B. Sonier Vinikoff. All authors: Department of Radiology, CHU Bretonneau, 37044 Tours, France. View all articles by this author. Philippe Rouleau.
Laurent Brunereau, Denis Herbreteau, and Philippe Rouleau. CHRU Bretonneau F.37044 Tours, France. We thank Dr. Kory for taking interest in our recent article , and we agree that figures 3B, 3C, 3D, and 3E did not accurately illustrate the reduction in size of the leiomyoma. In fact, in these figures we reported four sonographic views acquired ...
Romain Cailloce 1 , Elsa Tavernier 2 , Laurent Brunereau 3 , Adèle Fievet 1 , Céline Falip 1 , Fanny Dujardin 4 , Stéphanie Willot 5 , ... Université de Tours, Tours, France. [email protected]. PMID: 34100966 DOI: 10.1007/s00261-021-02960-w Abstract Purpose ...
Ureteropelvic junction (UPJ) obstruction is defined as an obstruction of the flow of urine from the renal pelvis to the proximal ureter. This results in high pressure in the renal pelvis, hydronephrosis, diminished renal function, and progressive renal damage. In its extreme form, UPJ obstruction may lead to complete loss of renal cortex.
Romain Cailloce 1 · Elsa T avernier 2 · Laurent Brunereau 3 · Adèle Fievet 1 · C éline Falip 1 · Fanny Dujardin 4 · ... CHRU de Tours, 49 Boule vard Beranger, 37000 Tours, France.
Emmanuelle Vermes 1 2 , Clémence Pantaléon 3 , Adrien Auvet 3 , Nicolas Cazeneuve 4 , Marie Christine Machet 5 , Anne Delhommais 4 , Thierry Bourguignon 3 , Michel Aupart 3 , Laurent Brunereau 4 Affiliations
Service de Radiologie Adulte, CHRU Tours, 37044, Tours cedex 9, France. Léo Ribier & Laurent Brunereau. Service de Chirurgie Maxillo-Faciale et Stomatologie, CHRU Tours, 37044, Tours cedex 9, France ... Laurent Brunereau. View author publications. You can also search for this author in PubMed Google ...
The authors are very grateful to Donam Kim, Jérôme Desoubeaux, and Kay Mc Carthy-Cerf from the Pedagogical Department of English learning in the Medical School of Tours University for their precious help with the English translation.
Laurent Brunereau Service de radiologie-neuroradiologie diagnostique et interventionnelle, CHU de Tours, Tours, Loire Valley, France. Search for more papers by this author
Twenty-three patients hospitalized in the Department of Ear, Nose and Throat at the University Hospital of Tours (France) were enrolled in this prospective study from January 2003 to December 2006. ... Radiology Department, CHU Bretonneau, Tours, France. Laurent Brunereau. Ear Nose and Throat Department, Bretonneau Hospital, Tours, France ...
Laurent Brunereau. Centre Hospitalier Universitaire de Tours; Philippe Bertrand. Philippe Bertrand. This person is not on ResearchGate, or hasn't claimed this research yet. ... Tours, France, from ...
Semantic Scholar extracted view of "Strategie de prise en charge des macrobiopsies mammaires au CHU de tours" by C. Vermersch et al. Skip to search form Skip to ... Ouldamer and G. Gabteni and J. M. Letourmy and Flavie Arbion and Henri Marret and Gilles Body and Franck Fetissof and Laurent Brunereau}, journal={Journal De Radiologie}, year={2006 ...
Laurent Brunereau MD, Radiology Department, CHU de Tours, Tours, France. Search for more papers by this author. Florence Cavé-Riant MD, Cryogenetics Laboratory, Hôpital Lariboisière, Assistance Publique-Hôpitaux de Paris. Search for more papers by this author. Florence Marchelli MD,
Background Pediatric magnetic resonance imaging (MRI) and computed tompgraphy (CT) require patient immobility and therefore often require sedation or general anesthesia of patients. Consensus on these procedures is lacking in France. Objective Thus, the aim of this study was to describe the current sedation practices for pediatric MRI and CT in France. Material and methods From January 2019 to ...
Purpose: Rapid prototyping is a technique used for creating computer images in three dimensions more efficiently than classic techniques. Percutaneous nephrolithotomy (PCNL) is a popular method to remove kidney stones; however, broader use by the urologic community has been hampered by the morbidity associated with needle puncture to gain access to the renal calix (bleeding, pneumothorax ...
The authors acknowledge Mr Jean Laurent Lasquellec for his invaluable technical support and Mr John Sheath for his English language assistance. Thanks to Marie Moinier, Madeleine and Capucine. ... CHRU de Tours, Tours, France. Laurent Brunereau & Frédéric Patat. Pathology, Tours University Hospital, University of Tours, Tours, France.
VIDÉO - Aujourd'hui, c'est au tour de Laurent Alexandre, entrepreneur spécialiste de l'IA, de faire face aux GG. - L'émission de libre expression sans filtre et sans masque social…