Does Medicare cover emergency room visits?
Published by Medicare Made Clear®

Yes, Medicare covers emergency room visits for injuries, sudden illnesses or an illness that gets worse quickly. Specifically, Medicare Part B will cover ER visits. And, since emergencies may occur anytime and anywhere, Medicare coverage for ER visits applies to any ER or hospital in the country. Note though, Medicare only covers emergency services in foreign countries in select situations.

How much does an ER visit cost?
Medicare typically charges a copay for each emergency room visit and copays for hospital services you receive during the visit. In addition to these copays, you will pay a coinsurance for doctor services you receive in the ER. Medicare Part B typically pays 80 percent of the Medicare-approved amount for doctor services, and you are responsible for the remaining 20 percent of the cost. The Part B deductible also applies.
The total amount you actually pay for an ER visit will depend on the type of facility you go to, whether you have other insurance, such as a Medicare supplement plan (Medigap) or a Medicare Advantage plan (Part C), and other factors.
Costs can change if you are admitted to the hospital
If an ER visit results in being you admitted to the hospital, then the visit is considered part of an inpatient stay and ER-related copays would not apply. To qualify as such, a hospital admission must happen within three days of the ER visit for the same or a related condition, and it must be at the hospital where ER services were provided. Admission to a different hospital within three days, even for the same condition, would be considered a separate event.
Does Medicare Advantage cover ER visits?
Medicare Advantage plans cover ER visits – and everything else that Original Medicare (Parts A & B) covers. By law, these plans must offer coverage equal to or better than what Original Medicare provides. So, though Medicare Advantage plans typically have provider networks, they must cover emergency care from both network and out-of-network providers. In other words, Medicare Advantage plans cover ER visits anywhere in the U.S.
Each Medicare Advantage plan sets its own cost terms for ER visits and other covered services. For example, you may pay copays or coinsurance for an ER visit and for services you receive while in the ER. Some plans also have deductibles. It’s important to check each plan’s details for information about coverage for ER visits.
About Medicare Made Clear
Medicare Made Clear brought to you by UnitedHealthcare provides Medicare education so you can make informed decisions about your health and Medicare coverage.
- Introduction to Medicare
- Types of plans
Get the latest
Boost your Medicare know-how with the reliable, up-to-date news and information delivered to your inbox every month.
*All fields required
More articles
Find a plan.
Enter your ZIP code for plans in your area
Call UnitedHealthcare toll-free at
1-833-301-2052, TTY 711
Hours: 8 a.m. - 8 p.m. 7 days a week
Meet with us
Make an appointment with a licensed insurance agent/producer in your area
Free webinar May 9: How to spot and stop a scam. Sign up now.
AARP daily Crossword Puzzle
Hotels with AARP discounts
Life Insurance
AARP Dental Insurance Plans
AARP MEMBERSHIP — $12 FOR YOUR FIRST YEAR WHEN YOU SIGN UP FOR AUTOMATIC RENEWAL
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
- right_container
Work & Jobs
Social Security
AARP en Español
- Membership & Benefits
AARP Rewards
- AARP Rewards %{points}%
Conditions & Treatments
Drugs & Supplements
Health Care & Coverage
Health Benefits

Staying Fit
Your Personalized Guide to Fitness

AARP Hearing Center
Ways To Improve Your Hearing

Brain Health Resources
Tools and Explainers on Brain Health

A Retreat For Those Struggling
Scams & Fraud
Personal Finance
Money Benefits

View and Report Scams in Your Area

AARP Foundation Tax-Aide
Free Tax Preparation Assistance

AARP Money Map
Get Your Finances Back on Track

How to Protect What You Collect
Small Business
Age Discrimination

Flexible Work
Freelance Jobs You Can Do From Home

AARP Skills Builder
Online Courses to Boost Your Career

31 Great Ways to Boost Your Career

ON-DEMAND WEBINARS
Tips to Enhance Your Job Search

Get More out of Your Benefits

When to Start Taking Social Security

10 Top Social Security FAQs

Social Security Benefits Calculator

Medicare Made Easy
Original vs. Medicare Advantage

Enrollment Guide
Step-by-Step Tool for First-Timers

Prescription Drugs
9 Biggest Changes Under New Rx Law

Medicare FAQs
Quick Answers to Your Top Questions
Care at Home
Financial & Legal
Life Balance

LONG-TERM CARE
Understanding Basics of LTC Insurance

State Guides
Assistance and Services in Your Area

Prepare to Care Guides
How to Develop a Caregiving Plan

End of Life
How to Cope With Grief, Loss
Recently Played
Word & Trivia
Atari® & Retro
Members Only
Staying Sharp
Mobile Apps
More About Games

Right Again! Trivia

Right Again! Trivia – Sports

Atari® Video Games

Throwback Thursday Crossword
Travel Tips
Vacation Ideas
Destinations
Travel Benefits

Beach vacation ideas
Vacations for Sun and Fun

Plan Ahead for Tourist Taxes

AARP City Guide
Discover Seattle

25 Ways to Save on Your Vacation
Entertainment & Style
Family & Relationships
Personal Tech
Home & Living
Celebrities
Beauty & Style

TV for Grownups
Best Reality TV Shows for Grownups

Robert De Niro Reflects on His Life

Looking Back
50 World Changers Turning 50

Sex & Dating
Spice Up Your Love Life

Navigate All Kinds of Connections

Life & Home
Couple Creates Their Forever Home

Store Medical Records on Your Phone?

Maximize the Life of Your Phone Battery

Virtual Community Center
Join Free Tech Help Events

Create a Hygge Haven

Soups to Comfort Your Soul

Your Ultimate Guide to Mulching
Driver Safety
Maintenance & Safety
Trends & Technology

AARP Smart Guide
How to Keep Your Car Running

We Need To Talk
Assess Your Loved One's Driving Skills

AARP Smart Driver Course

Building Resilience in Difficult Times

Tips for Finding Your Calm

Weight Loss After 50 Challenge

Cautionary Tales of Today's Biggest Scams

7 Top Podcasts for Armchair Travelers

Jean Chatzky: ‘Closing the Savings Gap’

Quick Digest of Today's Top News

AARP Top Tips for Navigating Life

Get Moving With Our Workout Series
You are now leaving AARP.org and going to a website that is not operated by AARP. A different privacy policy and terms of service will apply.
Go to Series Main Page
How does Medicare cover emergency room costs?
Kimberly Lankford,
The type of Medicare you have determines how it pays for emergency department services.
Original Medicare covers emergency services under Medicare Part B at any U.S. hospital or medical facility that accepts Medicare. However, that care is subject to a deductible and 20 percent copayment. Supplemental insurance, such as a Medigap policy or a retiree plan from your former employer, may cover these out-of-pocket expenses.

AARP Membership — $12 for your first year when you sign up for Automatic Renewal
Medicare defines an emergency as an injury, sudden illness or an illness that gets much worse.
If you’re admitted to the same hospital for a related condition within three days, you won’t have to pay the copayment because the visit is considered part of your inpatient hospital stay, covered through Medicare Part A .
Medicare Part B also covers urgent care visits needed to treat a sudden illness or injury that isn’t a medical emergency. Urgent care visits are also subject to a deductible and 20 percent copayment.
How does Medicare Advantage cover emergency services?
Medicare Advantage plans typically have provider networks and generally charge higher copayments and deductibles or don’t cover out-of-network care at all. But the rules are different for emergency services.
In this case, Medicare Advantage plans must cover emergency care as an in-network service, even if the hospital or facility isn’t in the provider’s network. But copayments may be different from under original Medicare.
For example, you may need to pay as much as a $135 copayment for each emergency room visit, whether it’s at an in-network or out-of-network facility. You can compare emergency care copayments for each Medicare Advantage plan in your area using the Medicare Plan Finder . Click on the Plan Details blue button at the bottom of an Advantage plan’s description.

AARP NEWSLETTERS

%{ newsLetterPromoText }%
%{ description }%
Privacy Policy
ARTICLE CONTINUES AFTER ADVERTISEMENT
A different definition of emergencies. For Advantage plans, the Centers for Medicare & Medicaid Services (CMS) considers an emergency medical condition one that, if not treated, could result in:
- Serious jeopardy to the health of the individual or, in the case of a pregnant woman, the health of the woman or her unborn child.
- Serious impairment to bodily functions.
- Serious dysfunction of any bodily organ or part.
Your emergency medical condition status is not affected if a later medical review found no actual emergency, CMS says. The plan can’t require prior authorization for emergency services.
AARP® Vision Plans from VSP™
Exclusive vision insurance plans designed for members and their families
With some MA plans, if you’re admitted to the hospital within 24 hours, you may not need to pay the copayment for the emergency room visit. Instead, it becomes part of your hospital stay.
How to find the details. Specifics vary by plan. See the plan summary on the website of each private plan or evidence of coverage. You can get to these documents through Medicare’s Plan Finder even if you’re not shopping for new coverage.
Log in if you have an account to see a summary of your current coverage. Or navigate through the Plan Finder by entering your zip code, choosing your coverage year, hitting the Continue button, clicking Medicare Advantage Plan (Part C) , tapping the Find Plans button and going though the questions. You don’t need to compare your drug costs, but you do want to get to the list of plans for your area and find your specific plan.
Click the Plan Details button, and on the next page the Plan website link. From there, your provider’s website will walk you through steps to learn information about your plan on its website. You’ll generally see a link to View plan summary or View plan documents within the plan information. Both documents are very detailed but often let you search within for “emergency” so you can find what’s relevant to your situation.
Urgent care also possible. Your Medicare Advantage plan may cover urgent care visits from out-of-network providers. These are nonemergency situations that require immediate medical attention when a network provider is not available, such as when you have a severe sore throat on a weekend and your doctor is off or if you’re traveling outside the plan’s service area.
You’ll have the same copayment as in-network urgent care, which could be around $50.

LEARN MORE ABOUT AARP MEMBERSHIP.
How does Medicare cover emergency ambulance services?
Medicare Part B covers emergency ambulance services , but they’re subject to a deductible and 20 percent coinsurance. A supplemental policy should help cover those.
Part B will pay for ambulance transportation to a hospital or skilled nursing facility if traveling in any other vehicle could endanger your health. This applies to emergency transport in an airplane or helicopter if you need immediate and rapid transport that a ground service can’t provide.
Medicare Advantage, too, covers emergency ambulance services, but like its emergency room coverage, its copay rates can be high. You may have a $300 copay for each one-way trip. See the plan’s evidence of coverage for details.
Keep in mind
Medicare covers emergency room visits throughout the United States, but it typically doesn’t cover emergency care outside the U.S., except in limited circumstances .
Some Medigap policies cover foreign travel emergency care with a lifetime limit of $50,000. Some Medicare Advantage plans provide limited coverage for foreign travel emergencies. Specifics vary a lot by plan.
Another option is buying travel insurance , which may provide more coverage for emergency care and medical evacuation when traveling.
Return to Medicare Q&A main page
Kimberly Lankford is a contributing writer who covers Medicare and personal finance. She wrote about insurance, Medicare, retirement and taxes for more than 20 years at Kiplinger’s Personal Finance and has written for The Washington Post and Boston Globe . She received the personal finance Best in Business award from the Society of American Business Editors and Writers and the New York State Society of CPAs’ excellence in financial journalism award for her guide to Medicare.
Discover AARP Members Only Access
Already a Member? Login

More on Medicare

How to Navigate the Emergency Department With an Older Adult

Care Tips to Keep Dementia Patients Safe at Home

What Forms Do I Need to Help With a Parent’s Health Care?
Caregivers should get signatures on these key documents
Recommended for You
AARP Value & Member Benefits

Learn, earn and redeem points for rewards with our free loyalty program

AARP® Dental Insurance Plan administered by Delta Dental Insurance Company
Dental insurance plans for members and their families

The National Hearing Test
Members can take a free hearing test by phone

AARP® Staying Sharp®
Activities, recipes, challenges and more with full access to AARP Staying Sharp®
SAVE MONEY WITH THESE LIMITED-TIME OFFERS
Medicare Interactive Medicare answers at your fingertips -->
Emergency room services, outpatient hospital services.
You must be logged in to bookmark pages.
Email Address * Required
Password * Required
Lost your password?
If you have Original Medicare , Part B covers emergency room services anywhere in the U.S. Medicare Advantage Plans also must cover emergency room services anywhere in the country. Emergency room services are typically provided when you have a medical condition that requires immediate action, such as an injury or sudden illness.
If you have a Medicare Advantage Plan, be aware that:
- Your plan cannot require you to see an in-network provider .
- You do not need a referral .
- There are limits on how much your plan can bill you if you receive emergency care while out of your plan’s network , Specifically, you will be billed either $50 or your plan’s in-network cost for emergency services, whichever is less.
- Your plan must cover medically necessary follow-up care related to the medical emergency if delaying care would endanger your health.
- You have the right to appeal if your plan does not cover your emergency care.
If your condition was not an emergency but appeared to be an emergency, Original Medicare or your Medicare Advantage Plan must still cover your care. For example, let’s say you have chest pain and think you are having a heart attack. If you go to the emergency room and doctors discover that your pain is heartburn, your care should still be covered because the situation appeared to be an emergency.
Even if you do not have health insurance or the ability to pay, you still have the right under federal law to receive medical care in the case of an emergency.
Update your browser to view this website correctly. Update my browser now
Does Medicare Cover Emergency Room Visits?

- by Christian Worstell
- January 12, 2024
- Reviewed by John Krahnert
Yes, emergency room visits are typically covered by Medicare .
Most outpatient emergency room services are covered by Medicare Part B, and inpatient hospital stays are covered by Medicare Part A.
Medicare Advantage plans (Part C) also cover ER visits . Many Medicare Advantage plans also offer benefits not found in Original Medicare.
Learn More About Medicare
Join our email series to receive your free Medicare guide and the latest information about Medicare and Medicare Advantage.
By clicking "Sign me up!” you are agreeing to receive emails from MedicareAdvantage.com.
Compare plans today.
Speak with a licensed insurance agent
1-800-557-6059 | TTY 711, 24/7
What Medicare Part A covers
Medicare Part A hospital insurance helps cover:
- Inpatient care in a hospital
- Skilled nursing facility care
- Hospice care
- Some home health care services
Medicare Part A is typically premium-free, as long as you or your spouse paid sufficient Medicare taxes while working.
If you go to the emergency room and are admitted as an inpatient , Medicare Part A helps cover some of the costs related to your hospital stay once your Part A deductible is met .
In 2024, the Medicare Part A deductible is $1,632 per benefit period .
What Medicare Part B covers
Medicare Part B is known as medical insurance and helps cover medically necessary services and preventive services, which can include:
- Doctor’s office visits
- Clinical research
- Ambulance services
- Durable medical equipment
- Mental health services
Medicare Part B may also cover services you receive when you visit the emergency room as an outpatient.
Medicare Part B is optional, and if you enroll in Part B you must also enroll in Part A. Unlike Medicare Part A, which is premium-free for most people, you must pay a monthly premium for Medicare Part B.
The standard Part B premium in 2024 is $174.70 per month.
Emergency room copayments and coinsurance
Even if your emergency room visit is covered by Medicare, you are typically responsible for paying a portion of the costs, known as copayments or coinsurance.
Typically, you pay a Medicare emergency room copayment for the visit itself and a copayment for each hospital service.
How you are charged depends on several factors, including which part of Medicare covers your visit (Medicare Part A, Medicare Part B or both) and whether or not you have met your Part A and Part B deductibles.
In 2024, the Part A deductible is $1,632 per benefit period, and the Part B deductible is $240 per year.
Medicare Part A coinsurance
Generally, if you go to the emergency room and are admitted as an inpatient, Medicare Part A will cover a portion of the costs, and in 2024 you pay:
- $0 coinsurance for each benefit period for days 1-60 spent in the hospital
- $408 coinsurance for days 61-90 in each benefit period
- $816 coinsurance per each “lifetime reserve day” beyond day 90 in each benefit period
- All costs beyond lifetime reserve days
Remember, you must meet your Part A deductible before Medicare will pay its share for covered services.
Medicare Part B copayments
If you go to the emergency room and receive care from a doctor but are not admitted as an inpatient, Medicare Part B will typically cover a portion of your medical costs.
After your Part B deductible is met, you typically pay 20 percent of the Medicare-approved amount for most services, and Medicare pays the rest.
Medicare Advantage plans cover emergency room visits
Medicare Advantage (Medicare Part C) is an alternative to Original Medicare (Medicare Part A and Part B) that provides the same hospital and medical benefits as Original Medicare. This means that Medicare Advantage plans, like Original Medicare, will cover at least some of your emergency room costs.
Most Medicare Advantage plans may also cover benefits not included in Medicare Part A or Part B.
To learn more about Medicare Advantage plans that may be available in your area and to find out about the emergency room coverage they offer, speak with a licensed insurance agent today.
Explore Medicare Advantage plan benefits in your area
Or call 1-800-557-6059 (TTY: 711) to speak with a licensed insurance agent. We accept calls 24/7!

About the author
Christian Worstell is a senior Medicare and health insurance writer with MedicareAdvantage.com. He is also a licensed health insurance agent. Christian is well-known in the insurance industry for the thousands of educational articles he’s written, helping Americans better understand their health insurance and Medicare coverage.
Christian’s work as a Medicare expert has appeared in several top-tier and trade news outlets including Forbes, MarketWatch, WebMD and Yahoo! Finance.
Christian has written hundreds of articles for MedicareAvantage.com that teach Medicare beneficiaries the best practices for navigating Medicare. His articles are read by thousands of older Americans each month. By better understanding their health care coverage, readers may hopefully learn how to limit their out-of-pocket Medicare spending and access quality medical care.
Christian’s passion for his role stems from his desire to make a difference in the senior community. He strongly believes that the more beneficiaries know about their Medicare coverage, the better their overall health and wellness is as a result.
A current resident of Raleigh, Christian is a graduate of Shippensburg University with a bachelor’s degree in journalism.
If you’re a member of the media looking to connect with Christian, please don’t hesitate to email our public relations team at [email protected] .

Related articles
Original Medicare (Parts A and B) doesn’t cover routine dental or vision care. 2024 Medicare Advantage (Part C) plans can cover benefits Original Medicare doesn’t cover, but dental and/or hearing benefits may not be available where you live. Learn more and find out how to compare the plans and benefits available in your area. Read more
Medicare Part B may cover emergency ambulance services, and some Medicare Advantage plans may offer non-emergency transportation to plan-approved locations. Learn more about Medicare transportation coverage. Read more
Medicare Advantage plans can offer gym memberships and fitness benefits that Original Medicare doesn’t cover, such as SilverSneakers. Learn how to compare your local plan options and how to find a Medicare Advantage plan that covers fitness benefits. Read more
While Original Medicare (Parts A and B) doesn’t cover hearing aids, Medicare Advantage (Part C) plans can cover hearing benefits Original Medicare doesn’t cover. Hearing benefits can be limited and may not be available where you live, so learn how to find out if Medicare Advantage plans that help pay for hearing aids are available in your area. Read more
Medicare Part B covers annual wellness visits. Medicare Advantage plans also cover annual wellness visits, and many Medicare Advantage plans also offer other wellness benefits not found in Original Medicare. Read more
Medicare Part A does not cover outpatient surgery, but Part B covers medically necessary outpatient surgery. Medicare Advantage plans may also cover outpatient surgery and include an annual out-of-pocket spending limit, which Original Medicare doesn’t offer. Read more
Original Medicare and Medicare Advantage plans can cover chiropractic care, but some plans may cover services more than others. Learn about what’s covered, what’s excluded and how much your Medicare costs could be. Read more
Medicare covers many telehealth services, and those benefits expanded during the coronavirus pandemic. Beneficiaries can use telehealth to access their doctor while also staying safe during COVID-19. Read more
Original Medicare (Medicare Parts A and B) doesn’t cover bathroom grab bars or other bathroom safety devices. Medicare Advantage plans can cover bathroom safety devices, but only in limited situations and only for beneficiaries who qualify. Read more

Join our email series to receive your Medicare guide and the latest information about Medicare.
Please enter your information to get your free quote.

Thanks for signing up for our emails!
Your Medicare guide will arrive in your email inbox shortly. You can also look forward to informative email updates about Medicare and Medicare Advantage.
If you'd like to speak with an agent right away, we're standing by for that as well. Give us a call!
Enter ZIP code
You're on your way to finding a Medicare Supplement plan!
Compare your Medigap plan options by visiting MedicareSupplement.com
Does Medicare Cover Emergency Room Visits?
Written by: Rachael Zimlich, RN, BSN
Reviewed by: Selah Lee, Licensed Insurance Agent
Key Takeaways
Original Medicare Original Medicare is a fee-for-service health insurance program available to Americans aged 65 and older and some individuals with disabilities. Original Medicare is provided by the federal government and is made up of two parts: Part A (hospital insurance) and Part B (medical insurance). will cover at least a portion of your visit to the emergency room.
The part of Medicare that covers your visit will depend on if you are admitted or not.
If you are admitted to the hospital for at least two nights after an ER visit, Medicare Part A covers it.
If you are not admitted after an ER visit, Medicare Part B will cover it.
How Much Does Medicare Pay for an Emergency Room Visit?
Original Medicare will cover a portion of your visits to the emergency room, but whether or not you are admitted will determine if Part A or Part B coverage is used. In either case, you pay a portion of your cost for services, but Medicare pays the majority.
If you have a Medicare Advantage plan, your ER visit will be covered and the plan you choose will determine your out-of-pocket costs. You may also have to pay more for visiting doctors or facilities that are outside your plan’s network.
Does Medicare Part A or B Cover Emergency Room Visits?
Both Medicare Part A and B offer some coverage of emergency services depending on how long you need to stay in the hospital. If your ER visit leads to a hospital stay, Medicare Part A covers the costs, plus any services that were provided in the three days before your admission. If your visit is one where you are discharged from the emergency room or after just one night of observation, Medicare Part B will provide coverage.
Will Medicare Part A Cover Emergency Room Visits?
Medicare Part A only covers emergency room services when you are admitted by a doctor for at least two nights in the hospital. The “Two-Midnight” rule is important, because in some cases your doctor may just keep you one night for observation. These visits are considered outpatient care even though you spent the night in the hospital, and Medicare Part B will provide coverage.
Medicare Part B covers most emergency visits, especially if you are seen and sent home the same day, or spend one night for observation. Even if you are admitted, Part B will pay the portion of your bill that covers doctor’s services while Part A will pay inpatient hospital costs.
Looking for dental, vision and hearing coverage?
Does Medicare Have a Copay for ER Visits?
Original Medicare does not have an established copay for emergency room visits. Instead, you will pay a share of the costs based on your Part A or Part B coverage, and which part of Medicare is applied to your visit.
If you are admitted for at least two nights after and ER visit and Part A is used, in 2024 you will pay:
- A $1,632 deductible for each inpatient stay for each benefit period. Benefit periods reset every 60 days you spend outside of a hospital or skilled nursing facility.
- If you were recently admitted and already paid this deductible for your benefit period, you will not have to pay it again for the same benefit period.
- Coinsurance applies, also, but only after 60 days of hospitalization.
If you visit the emergency room and are sent home right away or are admitted for just one night of observation, Part B coverage applies. This will cost you:
- Your annual deductible — $240 for 2024 — if you haven’t already met it for the year.
- Twenty percent of the remainder of the Medicare-approved costs associated with the visit.
How Much of a Hospital Bill Does Medicare Pay?
When Medicare Part A is applied for emergency department visits that turn into an inpatient stay, your costs will be covered after you pay your deductible and coinsurance.
When Medicare Part B is used for an ER visit where you are not admitted or kept only one night for observation, Medicare pays for 80% of the approved cost after your deductible is met.
Can I Get Help Paying?
If you need help paying for your share of your emergency department bill — regardless of whether Medicare Part A or B was applied — you may be able to use additional coverage if you’ve signed up for a Medicare supplement plan . Medicare supplement plans can only be purchased if you have Original Medicare (Parts A and B). If you have a Medicare Advantage plan, you will need to leave that policy.
Costs of Medicare supplement plans vary based on which plan you choose. Medicare supplement plans can be used to cover costs such as deductibles, copayments and coinsurance that are not covered by Original Medicare.
How Many ER Visits Does Medicare Cover?
There is no limit to how many ER visits Medicare covers, but you may have to start a new benefit period if it’s been awhile since your last admission. If you are admitted to the hospital and it’s been more than 60 days since your last admission, you will have to start a new benefit period and pay your Part A deductible. If you were admitted within the last 60 days, you will not have to pay this deductible again since you are in the same benefit period.
Find the Medicare Advantage plan that meets your needs.
Who Covers Ambulance Transportation?
Regardless of whether you are admitted or not following an ER visit, Medicare Part B is used to pay for ambulance services. If you’ve already met your Part B deductible for the year, you will be responsible for 20% of the cost of these services.
What About Medications?
Medications that you are given while admitted in the hospital are covered under Part A. If you are given a prescription in the emergency room and sent home, you will have to pay for this medication unless you have Medicare Part D coverage (prescription drug plans). Costs for prescription coverage vary based on the Medicare Part D plan you choose.
Have questions about your Medicare coverage?
Inpatient or outpatient hospital status affects your costs TRUSTED & VERIFIED medicare.gov . Medicare.gov.
Medicare costs at a glance . Medicare.gov.
This website is operated by GoHealth, LLC., a licensed health insurance company. The website and its contents are for informational and educational purposes; helping people understand Medicare in a simple way. The purpose of this website is the solicitation of insurance. Contact will be made by a licensed insurance agent/producer or insurance company. Medicare Supplement insurance plans are not connected with or endorsed by the U.S. government or the federal Medicare program. Our mission is to help every American get better health insurance and save money. Any information we provide is limited to those plans we do offer in your area. Please contact Medicare.gov or 1-800-MEDICARE to get information on all of your options.
Let's see if you're missing out on Medicare savings.
We just need a few details.
Related Articles

Skilled Nursing Facility
Medicare Skilled Nursing Facility (SNF) Coverage
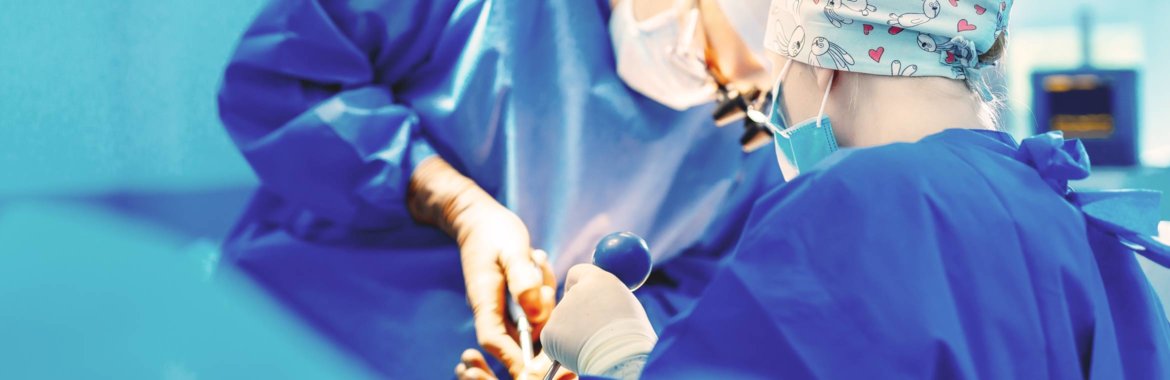
Weight Loss (Bariatric) Surgery
Does Medicare Cover Weight Loss or Bariatric Surgery?

Chemotherapy
Does Medicare Cover Chemotherapy? Understanding the Costs
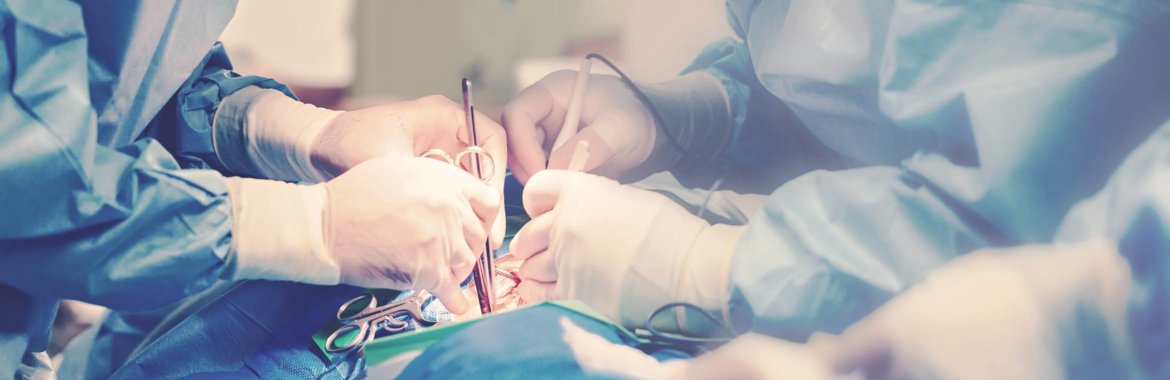
Does Medicare Cover Surgery?

Palliative Care
Does Medicare Cover Palliative Care?

Hospitals & Hospital Beds
Medicare Hospital Coverage

Does Medicare cover Hospice?

Home Health Care
Does Medicare Cover Home Health Care?
Let’s see if you qualify for Medicare savings today!
Speak with a Licensed Insurance Agent 877-388-0596 - TTY 711 (M-F 8am-9pm, Sat 9am-8pm EST)
Will Medicare Cover Emergency Room Visits?
Seniors account for more trips to the ER annually than any other age group. Falls, strokes, pain, and reactions to medications are just a few of the reasons people over the age of 65 visit the emergency room. Any trip to the emergency room can be stressful, but when you experience an injury, sudden illness, or medical event, you shouldn’t have to worry about the cost of the visit. If you are eligible for Medicare, you may get help paying for your trip to the ER.
Eligible for Medicare?
If you are 65 years of age or older, or have received Social Security benefits for 24 months, you will likely be automatically enrolled in premium-free Medicare Part A if you’ve paid Medicare taxes while working. When you first qualify for Medicare, you have the option of enrolling in Part B, or Medical Insurance. You pay a premium for Part B and will have a yearly deductible. Most Medicare recipients enroll in Part B during their Initial Enrollment Period to avoid paying late enrollment penalties. Part B benefits include coverage for doctor visits, preventive care, emergency department services under certain circumstances, and more.
How can Medicare help pay for your trip to the ER?
Anyone with Part B will be covered for trips to a hospital emergency room. You will pay a copayment for the emergency department visit and a copayment for each hospital service. You also pay 20% of the Medicare-approved amount for your doctor’s services and the Part B deductible applies. If you are admitted to the same hospital for a related condition within 3 days of your emergency department visit, you don’t pay the copayment because your visit is considered to be part of your inpatient stay.
Emergency services outside of the United States will only be covered in rare circumstances. If you travel abroad frequently and have Original Medicare, you may want to consider purchasing a Medigap policy. Medigap, also known as Medicare Supplement, policies may offer coverage for health services and supplies that you get outside of the United States. Medigap Plans C, D, G, M and N provide foreign travel emergency health care coverage.
Related articles
What is Medicare Parts A & B
New to Medicare
Medicare Advantage and Part D plans and benefits offered by the following carriers: Aetna Medicare, Anthem Blue Cross Blue Shield, Anthem Blue Cross, Aspire Health Plan, Cigna Healthcare, Dean Health Plan, Devoted Health, Florida Blue Medicare, GlobalHealth, Health Care Service Corporation, Healthy Blue, Humana, Molina Healthcare, Mutual of Omaha, Premera Blue Cross, Medica Central Health Plan, SCAN Health Plan, Scott and White Health Plan now part of Baylor Scott & White Health, Simply, UnitedHealthcare®, Wellcare, WellPoint
Need A Medicare Advantage Quote?
Request A Free Consultation For Medicare Advantage Plans
Does Medicare Cover Emergency Room Visits?

Yes, Medicare covers emergency room visits in a wide variety of circumstances. Medicare Part B covers emergency room visits for sudden illness, injuries, or other conditions that require immediate attention. If you’re admitted to the hospital from the emergency room, Medicare Part A covers your inpatient treatment and inpatient hospital stay .
Patients with Medicare Advantage may see additional benefits for ER visits, such as a set or waived copay .
Learn more about your expected share of costs for emergency room coverage as a Medicare beneficiary, and your alternative options if you need non-emergency care.
Table of Contents
Emergency room care a priority for older adults .
Emergency room visits are a medical necessity for many older adults. Falls are a leading cause of emergency room visits for older adults with Medicare in 2023, and other common reasons for emergency care include chest pain or stroke, car accidents, and heat-induced exhaustion. Medicare Part A and Part B, also called Original Medicare , works together to cover different aspects of emergency services for beneficiaries, ensuring access to necessary care.
When to Go to the Emergency Room
Emergency healthcare professionals use a tiered triage system to treat incoming patients by the severity of their condition. The above table illustrates a range of examples of when to go to the ER, from low-priority injuries or ailments (level 5) to life-threatening conditions (level 1).
The following urgent symptoms always warrant a trip to the ER:
- Chest pain or pressure
- Difficulty breathing or shortness of breath
- Severe abdominal pain or cramping
- Head injury or severe headache
- Seizures or loss of consciousness
- Severe burns or cuts
- Broken bones or dislocated joints
- Severe allergic reactions
- Signs of a stroke or heart attack
How Medicare Covers Emergency Room Visits
Emergency services may be covered by Medicare Part A or Part B, depending on the nature of the visit. While broad coverage in an emergency is guaranteed, it is important to understand which part covers which services, since you must meet your respective Part A and Part B deductibles before Medicare begins sharing costs for emergency services.
Overall Eligibility Criteria
For Medicare to pay for emergency room visits, beneficiaries must be experiencing a medical emergency that requires immediate attention. Coverage is not guaranteed for beneficiaries who visit the emergency room in a non-emergency situation. The emergency room facility must also accept Medicare.
How Medicare Part A Covers Emergency Services
Medicare Part A covers the following inpatient emergency services:
- Inpatient hospital care: Inpatient hospital care covered under Part A includes the cost of your stay in the hospital and any treatments required therein. Coverage includes general nursing, drugs used during your stay and specific to your reason for admission, and semi-private room accommodations. Part A benefits do not cover private rooms or private nursing services.
- Long-term hospital care: Once you pay your Part A deductible, Medicare covers a hospital stay of up to 60 days at no charge. After 60 days, you must pay coinsurance , or a portion of the cost, to continue your inpatient treatment.

Part A Coverage Criteria
Patients must be admitted to the same hospital where they visit the ER for at least two consecutive midnights to get coverage through Part A. So long as the patient is not admitted to the hospital, Part B pays for their care as an outpatient even if they spend the night in the emergency room.
How Medicare Part B Covers Emergency Services
Medicare Part B covers the following emergency outpatient services :
- Doctor care: Part B pays 80% of the costs of ambulatory care provided by a doctor in the ER, as long as you are not admitted to the hospital.
- Outpatient hospital care: Part B covers care provided to you in a hospital setting as an outpatient. Examples include overnight observation assessments, x-rays , and lab tests, and excludes medications you can administer yourself without the aid of a doctor.
- Emergency transportation: Emergencyambulance transportation to the nearest medical facility is covered under Part B, as long as the patient demonstrates that riding in any other vehicle would endanger their health, they are unconscious, or they require medical intervention during the ride. It may also be covered if you have a written order from your doctor stating the ambulance is medically necessary.
Part B Coverage Criteria
Medicare Part B covers outpatient services and routine medical care, including ambulatory care in the ER that does not require hospitalization. However, once you are admitted to the hospital, Part A covers your care.
How Medigap Covers ER Visits
Medigap offers supplemental coverage to help beneficiaries pay their Part A and Part B deductibles, copays, and coinsurance costs. You must have Original Medicare in place to purchase a Medigap plan from a private insurer.
Medigap may help cover your Part B deductible and the remaining 20% of ER costs that are your financial responsibility after Original Medicare pays for its share of costs.
How Medicare Advantage Covers ER Visits
Medicare Advantage is also known as Part C, and it offers the same coverage as Part A and Part B, but often with extras such as vision , dental , and hearing services. These plans are offered by private insurance companies approved by Medicare, so plan benefits, costs, and availability vary.
Medicare Advantage Plans are required to offer at least the same levels of coverage for emergency room visits as Original Medicare. However, the expanded benefits of many Part C plans may extend to ER services. For example, some MA Plans allow beneficiaries to waive their copay for an ER visit if they are admitted to the hospital within 24 hours, cutting down on costs due.
Medicare Advantage beneficiaries should review their policy to see how their plan covers emergency room visits, or speak with a trusted agent for more details.
How Much Does an ER Visit Cost Without Medicare?
The average ER visit cost $1,150 in 2020. Specifically, uninsured people paid an average of $2,188 for one or more visits to the ER that same year, with older people aged 45-64 paying even more at $2,243.
In contrast, Medicare beneficiaries pay either 20% of the approved care cost if they visit the emergency room once the Part B deductible is met, or the corresponding Part A copay if they are hospitalized once that deductible is met. This is often less expensive than paying for care out of pocket.
Alternatives For Medicare-Covered Care If You Do Not Have an Emergency
Medicare does not cover emergency room services if you are not experiencing a medical emergency. However, if you require non-critical but urgent medical attention, you may find the help you need through one of the following Medicare-covered ER alternatives:
- Urgent care clinics: Most urgent care clinics accept Medicare for the treatment of non-life-threatening but time-sensitive injuries or illnesses. Once you have met your Part B deductible, you are responsible for 20% of the cost of the urgent care visit. If you have not yet met the deductible, you may be responsible for paying out-of-pocket for this visit.
- Telehealth services : Medicare covers 80% of telehealth services under Part B as routine outpatient medical care. This is useful if you do not need hands-on treatment. For example, if you have a mental health emergency or need a healthcare provider to walk you through next steps, telehealth care can help. Like other Part B benefits, you must meet your deductible before Medicare pays their portion of this cost.
- Routine medical doctor’s appointment: Medicare also doctor appointments under Part B. If you can see your physician to address your emergency, this could be an ER alternative for care. You must meet your deductible in order for Medicare to pay 80% of this cost.
- Retail clinics: Medicare covers retail and other walk-in clinics under Part B, such as MinuteClinics inside CVS stores, RediClinics at Rite Aid, and Walmart Health Clinics. This could serve as an alternative for care if you have questions or concerns about medications. You must meet your deductible for Medicare to pay 80% of this cost.
Putting It All Together
The cost of accessing emergency medical services should never discourage someone from seeking help. This advice applies to everyone, regardless of their age or health status, but is especially relevant to Medicare beneficiaries who may require emergency room visits more frequently than the average person.
Medicare covers emergency services through Part B benefits, which include outpatient medical care. Beneficiaries who meet their Part B deductible owe 20% of ER costs, which includes treatment during their visit to the ER and ambulance transportation . Medicare also covers hospitalizations ordered by ER doctors and related expenses through Part A, should a patient require longer-term inpatient care.
You’re just a few steps away from seeing your Medicare Advantage plan options.
Inpatient or outpatient hospital status affects your costs
Your hospital status—whether you're an inpatient or an outpatient—affects how much you pay for hospital services (like X-rays , drugs , and lab tests ). Your hospital status may also affect whether Medicare will cover care you get in a skilled nursing facility (SNF) following your hospital stay.
- You're an inpatient starting when you're formally admitted to the hospital with a doctor's order. The day before you're discharged is your last inpatient day.
- You're an outpatient if you're getting emergency department services , observation services, outpatient surgery , lab tests, or X-rays, or any other hospital services, and the doctor hasn't written an order to admit you to a hospital as an inpatient. In these cases, you're an outpatient even if you spend the night in the hospital.
Observation services are hospital outpatient services you get while your doctor decides whether to admit you as an inpatient or discharge you. You can get observation services in the emergency department or another area of the hospital.
The decision for inpatient hospital admission is a complex medical decision based on your doctor’s judgment and your need for medically necessary hospital care. An inpatient admission is generally appropriate when you’re expected to need 2 or more midnights of medically necessary hospital care. But, your doctor must order such admission and the hospital must formally admit you in order for you to become an inpatient.
Each day you have to stay, you or your caregiver should always ask the hospital and/or your doctor, or a hospital social worker or patient advocate if you’re an inpatient or outpatient.
Here are some common hospital situations and a description of how Medicare will pay. Remember, you pay your deductible , coinsurance, and copayment .
Remember, even if you stay overnight in a regular hospital bed, you might be an outpatient. Ask the doctor or hospital. If you have a Medicare Advantage Plan, your costs and coverage may be different. Check with your plan.
You may get a Medicare Outpatient Observation Notice (MOON) that lets you know you’re an outpatient in a hospital or critical access hospital. You must get this notice if you're getting outpatient observation services for more than 24 hours. The MOON will tell you why you’re an outpatient getting observation services, instead of an inpatient. It will also let you know how this may affect what you pay while in the hospital, and for care you get after leaving the hospital.
The copayment for a single outpatient hospital service can’t be more than the inpatient hospital deductible. However, your total copayment for all outpatient services may be more than the inpatient hospital deductible.
- Skip to main content
- Keyboard shortcuts for audio player
- Your Health
- Treatments & Tests
- Health Inc.
- Public Health
Medicare's push to improve chronic care attracts businesses, but not many doctors
Phil Galewitz
Holly K. Hacker

Medicare enrollees with two or more chronic conditions are eligible for Chronic Care Management, which pays doctors to check in with those patients monthly. But the service hasn't caught on. John Moore/Getty Images hide caption
Medicare enrollees with two or more chronic conditions are eligible for Chronic Care Management, which pays doctors to check in with those patients monthly. But the service hasn't caught on.
Carrie Lester looks forward to the phone call every Thursday from her doctors' medical assistant, who asks how she's doing and if she needs prescription refills. The assistant counsels her on dealing with anxiety and her other health issues.
Lester credits the chats for keeping her out of the hospital and reducing the need for clinic visits to manage chronic conditions including depression, fibromyalgia and hypertension.
"Just knowing someone is going to check on me is comforting," says Lester, 73, who lives with her dogs, Sophie and Dolly, in Independence, Kansas.
At least two-thirds of Medicare enrollees have two or more chronic health conditions, federal data shows . That makes them eligible for a federal program that, since 2015, has rewarded doctors for doing more to manage their health outside office visits.
But while early research found the service, called Chronic Care Management, reduced emergency room and in-patient hospital visits and lowered total health spending, uptake has been sluggish.
Federal data from 2019 shows just 4% of potentially eligible enrollees participated in the program, a figure that appears to have held steady through 2023, according to a Mathematica analysis. About 12,000 physicians billed Medicare under the CCM mantle in 2021, according to the latest Medicare data analyzed by KFF Health News. (The Medicare data includes doctors who have annually billed CCM at least a dozen times.)
By comparison, federal data shows about 1 million providers participate in Medicare.
$62 per patient, per month
Even as the strategy has largely failed to live up to its potential, thousands of physicians have boosted their annual pay by participating, and auxiliary for-profit businesses have sprung up to help doctors take advantage of the program. The federal data showed about 4,500 physicians received at least $100,000 each in CCM pay in 2021.
Through the CCM program, Medicare pays to develop a patient care plan, coordinate treatment with specialists, and regularly check in with beneficiaries. Medicare pays doctors a monthly average of $62 per patient , for 20 minutes of work with each, according to companies in the business.
Without the program, providers often have little incentive to spend time coordinating care because they can't bill Medicare for such services.
Health policy experts say a host of factors limit participation in the program. Chief among them is that it requires both doctors and patients to opt in. Doctors may not have the capacity to regularly monitor patients outside office visits. Some also worry about meeting the strict Medicare documentation requirements for reimbursement and are reluctant to ask patients to join a program that may require a monthly copayment if they don't have a supplemental policy.
"This program had potential to have a big impact," says Kenneth Thorpe , an Emory University health policy expert on chronic diseases. "But I knew it was never going to work from the start because it was put together wrong."
He said most doctor's offices are not set up for monitoring patients at home. "This is very time-intensive and not something physicians are used to doing or have time to do," Thorpe says.
For patients, the CCM program is intended to expand the type of care offered in traditional, fee-for-service Medicare to match benefits that — at least in theory — they may get through Medicare Advantage, which is administered by private insurers.
But the CCM program is open to both Medicare and Medicare Advantage beneficiaries.
The program was also intended to boost pay to primary care doctors and other physicians who are paid significantly less by Medicare than specialists, says Mark Miller, a former executive director of the Medicare Payment Advisory Commission, which advises Congress. He's currently an executive vice president of Arnold Ventures, a philanthropic organization focused on health policy. (The organization has also provided funding for KFF Health News .)
Not "easy money"
Despite the allure of extra money, some physicians have been put off by the program's upfront costs.
"It may seem like easy money for a physician practice, but it is not," says Dr. Namirah Jamshed, a physician at UT Southwestern Medical Center in Dallas.
Jamshed says the CCM program was cumbersome to implement because her practice was not used to documenting time spent with patients outside the office, a challenge that included finding a way to integrate the data into electronic health records. Another challenge was hiring staff to handle patient calls before her practice started getting reimbursed by the program.
Only about 10% of the practice's Medicare patients are enrolled in CCM, she says.
Jamshed says her practice has been approached by private companies looking to do the work, but the practice demurred out of concerns about sharing patients' health information and the cost of retaining the companies. Those companies can take more than half of what Medicare pays doctors for their CCM work.
Dr. Jennifer Bacani McKenney, who runs a family medicine practice in Fredonia, Kansas, with her father — where Carrie Lester is a patient — says the CCM program has worked well.
She says having a system to keep in touch with patients at least once a month has reduced their use of emergency rooms — including for some who were prone to visits for nonemergency reasons, such as running out of medication or even feeling lonely. The CCM funding enables the practice's medical assistant to call patients regularly to check in, something it could not afford before.
For a small practice, having a staffer who can generate extra revenue makes a big difference, McKenney says.
While she estimates about 90% of their patients would qualify for the program, only about 20% are enrolled. One reason is that not everyone needs or wants the calls, she says.
While the program has captured interest among internists and family medicine doctors, it has also paid out hundreds of thousands of dollars to specialists, such as those in cardiology, urology and gastroenterology, the KFF Health News analysis finds. Primary care doctors are often seen as the ones who coordinate patient care, making the payments to specialists notable.
A federally funded study by Mathematica in 2017 found the CCM program saves Medicare $74 per patient per month, or $888 per patient per year — due mostly to a decreased need for hospital care.
The study quoted providers who were unhappy with attempts to outsource CCM work. "Third-party companies out there turn this into a racket," the study cites one physician saying, noting that companies employ nurses who don't know patients.
Nancy McCall, a Mathematica researcher who co-authored the 2017 study, says doctors are not the only resistance point. "Patients may not want to be bothered or asked if they are exercising or losing weight or watching their salt intake," she says.
How outsourcing works
Still, some physician groups say it's convenient to outsource the program.
UnityPoint Health, a large integrated health system based in Iowa, tried doing chronic care management on its own, but found it administratively burdensome, says Dawn Welling, the UnityPoint Clinic's chief nursing officer.
For the past year, it has contracted with a Miami-based company, HealthSnap, to enroll patients, have its nurses make check-in calls each month, and help with billing. HealthSnap helps manage care for more than 16,000 of UnityPoint Health's Medicare patients — a small fraction of its Medicare patients, which includes those enrolled in Medicare Advantage.
Some doctors were anxious about sharing patient records and viewed the program as a sign they weren't doing enough for patients, Welling says. But she says the program has been helpful, particularly to many enrollees who are isolated and need help changing their diet and other behaviors to improve health.
"These are patients who call the clinic regularly and have needs, but not always clinical needs," Welling says.
Samson Magid, CEO of HealthSnap, says more doctors have started participating in CCM since Medicare increased pay in 2022 for 20 minutes of work, to $62 from $41, and added billing codes for additional time.
To help ensure patients pick up the phone, caller ID shows HealthSnap calls as coming from their doctor's office, not from wherever the company's nurse might be located. The company also hires nurses from different regions so they may speak with dialects similar to those of the patients they work with, Magid says.
He says some enrollees have been in the program for three years and many could stay enrolled for life, which means they can bill patients and Medicare long-term.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF — the independent source for health policy research, polling, and journalism.
- Centers for Medicare & Medicaid Services
- primary care

Here's what 'young seniors' need to know to get ahead of navigating Medicare
M ore than 4 million Americans will turn 65 this year, which means they will have to navigate a new health care journey: Medicare , according to a report from the Alliance for Lifetime Income.
Adults turning 65 years old this year have much to consider when choosing a Medicare plan and provider, from evaluating current health care needs to anticipating changing life situations.
Frankly, the process can be a little daunting, so where should they begin?
Here's what “young seniors” need to know to get ahead of this new milestone.
To let us know how WCNC Charlotte can help you get ahead in 2024, email us at [email protected] .
"Medicare is what we've paid into our whole lives while we were working," Dr. Jennifer Taylor, the lead medical director at Humana , said. "Then when we turn 65, we are entitled to that care, which is sponsored through the government."
Taylor said it’s important for older adults to start their research now.
"It's really important to understand all the different parts of Medicare, so you can make a decision based on your own individual needs," she said.
Taylor said there’s the traditional Medicare plan, which covers hospital visits and ER visits, but added those have a deductible.
"You also can buy a plan called a Part D plan that covers your prescriptions," Taylor said.
⏯ Subscribe to WCNC Charlotte on YouTube to be notified of new videos
She said while anyone at any age should have a primary care doctor, that’s absolutely imperative for older adults.
"Because having a doctor that knows you, your own personal history and your own individual health needs, [that] can make a real difference in terms of your quality of life and your longevity," she said.
Also, make sure you know all that your Medicare plan can do for you, so you can maximize your benefits and stay healthy.
"It's super important to understand your benefits," she explained " Medicare Part B , for example, offers a lot of things that you might not even be aware of, like help with tobacco cessation, or help if you have a problem with alcohol."
Check to find the Medicare plan that works best for you.
WCNC Charlotte's Where's The Money series is all about leveling the playing field in the Carolinas by helping others and breaking down barriers. WCNC Charlotte doesn't want our viewers to be taken advantage of, so we’re here to help. Watch previous stories where we ask the question “Where’s the Money” in the YouTube playlist below and subscribe to get updated when new videos are uploaded.

Updated research request forms and data security approval requirement effective 4/24/23

- A-Z Glossary
Our site will be undergoing a maintenance update on Wednesday, August 4th from 8am-12pm CT . You may experience up to 10 minutes of downtime during the update.
In light of the evolving COVID-19 situation, we want to assure you that ResDAC is open for business . We are actively responding to all phone and email inquiries.
- Find CMS Data Files
- Request CMS Data Files
- Search Data Variables
- Learn About CMS Data
How to Identify Hospital Claims for Emergency Room Visits in the Medicare Claims Data
This article provides guidance on how to identify hospital emergency room claims from the Medicare files.
Hospitals submit claims containing ER services on a CMS-1450 form (aka UB-04). Their claims containing ER charges will be found in the inpatient claims data (Inpatient file or MedPAR file) and the outpatient claims file.
Claims in the Outpatient and Inpatient files are identified via Revenue Center Code values of 0450-0459 (Emergency room) or 0981 (Professional fees-Emergency room).
Claims in the MedPAR file are identified via the Emergency Room Charge Amount field when the amount is > $0.
Although one can assume ER patients found in the inpatient data were admitted to the hospital, one cannot assume ER patients found in the outpatient data were not admitted to the hospital. Because some patients are transferred to a different hospital for admission and some hospitals bill ER and inpatient services separately, determining admission status for those ER visits found in the Outpatient file requires linking to the inpatient data to find evidence of an admission.
Please note charges for one ER visit will be found in either the Outpatient claims or the Inpatient claims; a visit will not generate ER charges on both an inpatient claim and an outpatient claim.
In summary, to find ER visits:
- Outpatient files: Revenue Center Codes 0450-0459, 0981
- Inpatient files: Revenue Center Codes 0450-0459, 0981
- Inpatient MedPAR: Emergency Room Charge Amount > $0
Note regarding LDS data: The MedPAR Hospital National LDS file does not include a beneficiary-level identifier and cannot be linked to other data files, including the Outpatient SAF LDS. The Inpatient SAF LDS and Outpatient SAF LDS files are necessary to identify all ER visits that resulted in a hospital stay when working with the LDS data. RIF MedPAR files do contain beneficiary identifiers and can be linked to other RIF claims files.
Article Information
- Alzheimer's disease & dementia
- Arthritis & Rheumatism
- Attention deficit disorders
- Autism spectrum disorders
- Biomedical technology
- Diseases, Conditions, Syndromes
- Endocrinology & Metabolism
- Gastroenterology
- Gerontology & Geriatrics
- Health informatics
- Inflammatory disorders
- Medical economics
- Medical research
- Medications
- Neuroscience
- Obstetrics & gynaecology
- Oncology & Cancer
- Ophthalmology
- Overweight & Obesity
- Parkinson's & Movement disorders
- Psychology & Psychiatry
- Radiology & Imaging
- Sleep disorders
- Sports medicine & Kinesiology
- Vaccination
- Breast cancer
- Cardiovascular disease
- Chronic obstructive pulmonary disease
- Colon cancer
- Coronary artery disease
- Heart attack
- Heart disease
- High blood pressure
- Kidney disease
- Lung cancer
- Multiple sclerosis
- Myocardial infarction
- Ovarian cancer
- Post traumatic stress disorder
- Rheumatoid arthritis
- Schizophrenia
- Skin cancer
- Type 2 diabetes
- Full List »
share this!
April 23, 2024
This article has been reviewed according to Science X's editorial process and policies . Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
reputable news agency
Medicare's push to improve chronic care attracts businesses, but not many doctors
by Phil Galewitz, KFF Health News, Holly K. Hacker, KFF Health News

At least two-thirds of Medicare enrollees have two or more chronic health conditions, federal data shows. That makes them eligible for a federal program that, since 2015, has rewarded doctors for doing more to manage their health outside office visits.
But while early research found the service, called Chronic Care Management, reduced emergency room and in-patient hospital visits and lowered total health spending, uptake has been sluggish.
Federal data from 2019 shows just 4% of potentially eligible enrollees participated in the program, a figure that appears to have held steady through 2023, according to a Mathematica analysis. About 12,000 physicians billed Medicare under the CCM mantle in 2021, according to the latest Medicare data analyzed by KFF Health News. (The Medicare data includes doctors who have annually billed CCM at least a dozen times.)
By comparison, federal data shows about 1 million providers participate in Medicare.
Even as the strategy has largely failed to live up to its potential, thousands of physicians have boosted their annual pay by participating, and auxiliary for-profit businesses have sprung up to help doctors take advantage of the program. The federal data showed about 4,500 physicians received at least $100,000 each in CCM pay in 2021.
Through the CCM program, Medicare pays to develop a patient care plan, coordinate treatment with specialists, and regularly check in with beneficiaries. Medicare pays doctors a monthly average of $62 per patient, for 20 minutes of work with each, according to companies in the business.
Without the program, providers often have little incentive to spend time coordinating care because they can't bill Medicare for such services.
Health policy experts say a host of factors limit participation in the program. Chief among them is that it requires both doctors and patients to opt in. Doctors may not have the capacity to regularly monitor patients outside office visits. Some also worry about meeting the strict Medicare documentation requirements for reimbursement and are reluctant to ask patients to join a program that may require a monthly copayment if they don't have a supplemental policy.
"This program had potential to have a big impact," said Kenneth Thorpe, an Emory University health policy expert on chronic diseases. "But I knew it was never going to work from the start because it was put together wrong."
He said most doctors' offices are not set up for monitoring patients at home. "This is very time-intensive and not something physicians are used to doing or have time to do," Thorpe said.
For patients, the CCM program is intended to expand the type of care offered in traditional, fee-for-service Medicare to match benefits that—at least in theory—they may get through Medicare Advantage, which is administered by private insurers.
But the CCM program is open to both Medicare and Medicare Advantage beneficiaries.
The program was also intended to boost pay to primary care doctors and other physicians who are paid significantly less by Medicare than specialists, said Mark Miller, a former executive director of the Medicare Payment Advisory Commission, which advises Congress. He's currently an executive vice president of Arnold Ventures, a philanthropic organization focused on health policy.
Despite the allure of extra money, some physicians have been put off by the program's upfront costs.
"It may seem like easy money for a physician practice, but it is not," said Namirah Jamshed, a physician at UT Southwestern Medical Center in Dallas.
Jamshed said the CCM program was cumbersome to implement because her practice was not used to documenting time spent with patients outside the office, a challenge that included finding a way to integrate the data into electronic health records. Another challenge was hiring staff to handle patient calls before her practice started getting reimbursed by the program.
Only about 10% of the practice's Medicare patients are enrolled in CCM, she said.
Jamshed said her practice has been approached by private companies looking to do the work, but the practice demurred out of concerns about sharing patients' health information and the cost of retaining the companies. Those companies can take more than half of what Medicare pays doctors for their CCM work.
Physician Jennifer Bacani McKenney, who runs a family medicine practice in Fredonia, Kansas, with her father—where Carrie Lester is a patient—said the CCM program has worked well.
She said having a system to keep in touch with patients at least once a month has reduced their use of emergency rooms—including for some who were prone to visits for nonemergency reasons, such as running out of medication or even feeling lonely. The CCM funding enables the practice's medical assistant to call patients regularly to check in, something it could not afford before.
For a small practice, having a staffer who can generate extra revenue makes a big difference, McKenney said.
While she estimates about 90% of their patients would qualify for the program, only about 20% are enrolled. One reason is that not everyone needs or wants the calls, she said.
While the program has captured interest among internists and family medicine doctors, it has also paid out hundreds of thousands of dollars to specialists, such as those in cardiology, urology, and gastroenterology, the KFF Health News analysis found. Primary care doctors are often seen as the ones who coordinate patient care, making the payments to specialists notable.
A federally funded study by Mathematica in 2017 found the CCM program saves Medicare $74 per patient per month, or $888 per patient per year—due mostly to a decreased need for hospital care.
The study quoted providers who were unhappy with attempts to outsource CCM work. "Third-party companies out there turn this into a racket," the study cited one physician as saying, noting companies employ nurses who don't know patients.
Nancy McCall, a Mathematica researcher who co-authored the 2017 study, said doctors are not the only resistance point. "Patients may not want to be bothered or asked if they are exercising or losing weight or watching their salt intake," she said.
Still, some physician groups say it's convenient to outsource the program.
UnityPoint Health, a large integrated health system based in Iowa, tried doing chronic care management on its own, but found it administratively burdensome, said Dawn Welling, the UnityPoint Clinic's chief nursing officer.
For the past year, it has contracted with a Miami-based company, HealthSnap, to enroll patients, have its nurses make check-in calls each month, and help with billing. HealthSnap helps manage care for over 16,000 of UnityHealth's Medicare patients—a small fraction of its Medicare patients, which includes those enrolled in Medicare Advantage.
Some doctors were anxious about sharing patient records and viewed the program as a sign they weren't doing enough for patients, Welling said. But she said the program has been helpful, particularly to many enrollees who are isolated and need help changing their diet and other behaviors to improve health.
"These are patients who call the clinic regularly and have needs, but not always clinical needs," Welling said.
Samson Magid, CEO of HealthSnap, said more doctors have started participating in the CCM program since Medicare increased pay in 2022 for 20 minutes of work, to $62 from $41, and added billing codes for additional time.
To help ensure patients pick up the phone, caller ID shows HealthSnap calls as coming from their doctor's office, not from wherever the company's nurse might be located. The company also hires nurses from different regions so they may speak with dialects similar to those of the patients they work with, Magid said.
He said some enrollees have been in the program for three years and many could stay enrolled for life—which means they can bill patients and Medicare long-term.
2024 KFF Health News. Distributed by Tribune Content Agency, LLC.
Explore further
Feedback to editors

Research shows 'profound' link between dietary choices and brain health
11 hours ago

Component of keto diet plus immunotherapy may reduce prostate cancer
15 hours ago

Study finds big jump in addiction treatment at community health clinics

Positive childhood experiences can boost mental health and reduce depression and anxiety in teens

Gene linked to epilepsy and autism decoded in new study
Apr 26, 2024

Blood test finds knee osteoarthritis up to eight years before it appears on X-rays

Researchers find pregnancy cytokine levels impact fetal brain development and offspring behavior

Study finds biomarkers for psychiatric symptoms in patients with rare genetic condition 22q

Clinical trial evaluates azithromycin for preventing chronic lung disease in premature babies

Scientists report that new gene therapy slows down amyotrophic lateral sclerosis disease progression
Related stories.
COVID and Medicare payments spark remote patient BP monitoring boom
Mar 28, 2024
Hospitals can care for Medicare patients at home in pandemic
Nov 25, 2020
Sicker Americans are sticking with Medicare managed care plans, study finds
Jun 27, 2023

The importance of telehealth for Medicare beneficiaries during the COVID-19 pandemic
Nov 17, 2021
Medicare proposes to pay docs for analyzing texted photos
Jul 13, 2018

Study: Prevention suffers when doctors drop out of Medicare's ACO program
Feb 8, 2022
Recommended for you

Homelessness found to be a major issue for many patients in the emergency department

Proposed changes to Medicare, Medicaid could cost thousands of lives, study finds
Apr 23, 2024

Most acute care hospitals do not admit representative proportion of Black Medicare patients in their local market: Study

Chronic pain linked to socioeconomic background
Apr 22, 2024

A study in Brazil shows social programs have prevented 1.4 million all-age deaths over the past two decades

Taking a leave of absence can harm medical students' match prospects, finds study
Apr 16, 2024
Let us know if there is a problem with our content
Use this form if you have come across a typo, inaccuracy or would like to send an edit request for the content on this page. For general inquiries, please use our contact form . For general feedback, use the public comments section below (please adhere to guidelines ).
Please select the most appropriate category to facilitate processing of your request
Thank you for taking time to provide your feedback to the editors.
Your feedback is important to us. However, we do not guarantee individual replies due to the high volume of messages.
E-mail the story
Your email address is used only to let the recipient know who sent the email. Neither your address nor the recipient's address will be used for any other purpose. The information you enter will appear in your e-mail message and is not retained by Medical Xpress in any form.
Newsletter sign up
Get weekly and/or daily updates delivered to your inbox. You can unsubscribe at any time and we'll never share your details to third parties.
More information Privacy policy
Donate and enjoy an ad-free experience
We keep our content available to everyone. Consider supporting Science X's mission by getting a premium account.
E-mail newsletter
The Federal Register
The daily journal of the united states government, request access.
Due to aggressive automated scraping of FederalRegister.gov and eCFR.gov, programmatic access to these sites is limited to access to our extensive developer APIs.
If you are human user receiving this message, we can add your IP address to a set of IPs that can access FederalRegister.gov & eCFR.gov; complete the CAPTCHA (bot test) below and click "Request Access". This process will be necessary for each IP address you wish to access the site from, requests are valid for approximately one quarter (three months) after which the process may need to be repeated.
An official website of the United States government.
If you want to request a wider IP range, first request access for your current IP, and then use the "Site Feedback" button found in the lower left-hand side to make the request.
Supreme Court wrestles with abortion clash over emergency room treatment for pregnant women
WASHINGTON — The Supreme Court appeared divided Wednesday as it grappled with whether provisions of Idaho's near-total abortion ban unlawfully conflict with a federal law aimed at ensuring certain standards for emergency medical care for patients, including pregnant women.
Some conservative justices, who have a 6-3 majority, appeared skeptical about the Biden administration’s lawsuit arguing that the state ban restricts potentially lifesaving treatment for women suffering complications during pregnancy.
Liberal members of the court appeared to back the administration's position.
The justices are weighing an appeal brought by Idaho officials who are contesting a lawsuit the Biden administration filed over abortion access in emergency situations.

The state abortion law was enacted in 2020, with a provision stating it would go into effect if the Supreme Court overturned Roe v. Wade, the 1973 ruling that found women had a constitutional right to abortion.
The 2020 law, called the Defense of Life Act, went into effect in 2022 when the Supreme Court rolled back Roe.
The state law says anyone who performs an abortion is subject to criminal penalties, including up to five years in prison. Health care professionals found to have violated the law can lose their professional licenses.
The federal government sued, leading a federal judge in August 2022 to block the state from enforcing provisions concerning medical care that is required under the federal Emergency Medical Treatment and Labor Act, or EMTALA.
The federal law, enacted in 1986, requires that patients receive appropriate emergency room care. The Biden administration argues that care should include abortions in certain situations. The law applies to any hospital that receives federal funding under the Medicare program.
There is an exception to the Idaho law if an abortion is necessary to protect the life of the pregnant woman, although the scope of the exception came under close scrutiny during the oral argument.
Idaho’s lawyer, Joshua Turner, faced tough questioning about whether the exception can also apply to a situation in which a woman has complications that pose a substantial health risk but not imminent death.
Liberal Justice Elena Kagan said federal law says “that you don’t have to wait until the person is on the verge of death.”
“If the woman is going to lose her reproductive organs, that’s enough to trigger this duty on the part of the hospital to stabilize the patient,” she said.
Fellow liberal Justice Sonia Sotomayor asked similar questions, providing several examples of real-life situations in which women have faced emergency situations when doctors had to make calls about whether to authorize abortions, including a situation in which a patient at 16 weeks of pregnancy whose water broke was at risk of sepsis or a hemorrhage after she was refused an abortion in Florida.
"Is that a case in which Idaho the day before would have said it's OK to have an abortion?" Sotomayor asked.
Turner argued that such medical decisions are “subjective” and that a doctor’s judgment in such instances would be based on good faith, not an objective standard.
Justices Amy Coney Barrett and Brett Kavanaugh, both conservatives, indicated they saw Idaho’s law as allowing for treatment similar to what the Biden administration says the federal law requires, suggesting that there may not be any conflict.
At one point Barrett said she was "shocked" at Turner's answers to questions about what kind of treatment was allowed, because "I thought your own expert had said below that these kinds of cases were covered."
Kavanaugh likewise questioned the daylight between the two laws, wondering what the implications are if "Idaho law allows an abortion in each of the emergency circumstances that is identified by the government."
"What does that mean for what we're deciding here?" he asked Turner.
Conservative Justice Samuel Alito seemed most skeptical of the federal government's argument, at one point mentioning language in the federal law referring to treatment for an "unborn child," a term more commonly used by anti-abortion advocates.
"Isn't that an odd phrase to put in a statute that imposes a mandate to perform abortions?" Alito asked Solicitor General Elizabeth Prelogar.
"Have you seen abortion statutes that use the phrase 'unborn child'? Doesn't that tell us something?"
Prelogar responded that the phrase did not displace the requirement that women get the treatment they need in emergency situations.
Conservative justices, including Neil Gorsuch, also questioned whether the federal government even has the power to mandate health standards when they are tied to Medicare funding.
In January, the Supreme Court allowed Idaho to enforce the provisions while also agreeing to hear oral arguments in the case. Other provisions of the ban are already in effect and will not be affected by how the justices rule.
The decision will affect not just Idaho but also other states, including Texas, that have enacted similar abortion bans that abortion-rights advocates say clash with the federal law.
In blocking parts of the state law that conflict with federal law, U.S. District Court Judge B. Lynn Winmill described the state’s actions as putting doctors in a difficult situation.
“The doctor believes her EMTALA obligations require her to offer that abortion right now. But she also knows that all abortions are banned in Idaho. She thus finds herself on the horns of a dilemma. Which law should she violate?” he wrote.
The San Francisco-based 9th U.S. Circuit Court of Appeals briefly put Winmill’s ruling on hold in September, but it subsequently allowed it to go back into effect, prompting the state officials to turn to the Supreme Court.
Prelogar wrote in court papers that EMTALA requires "necessary stabilizing treatment," which in cases involving pregnant women in emergency situations may require abortions.
"And in those limited but critically important circumstances EMTALA requires the hospital to offer that care," she added.
The state argues that it was only after Roe was overturned that the Biden administration said EMTALA could be interpreted to require abortions in some contexts, calling it a "nationwide abortion mandate."
EMTALA "merely prohibits emergency rooms from turning away indigent patients with serious medical conditions," Idaho Attorney General Raúl Labrador wrote in court papers. The law was not intended to override state laws regulating health care, he added.
The Idaho dispute is one of two abortion cases now pending at the Supreme Court, both of which arose in the aftermath of the 2022 decision to overturn Roe v. Wade. In the other case, the court is considering a challenge that could restrict access to mifepristone, the drug most commonly used for medication abortions.
Lawrence Hurley covers the Supreme Court for NBC News.

IMAGES
VIDEO
COMMENTS
A copayment is a fixed amount, like $30. for each emergency department visit and a copayment for each hospital service you get. After you meet the Part B. deductible. Deductible. The amount you must pay for health care or prescriptions before Original Medicare, your Medicare Advantage Plan, your Medicare drug plan, or your other insurance ...
1-833-301-2052, TTY 711. Hours: 8 a.m. - 8 p.m. 7 days a week. Find an Agent. Medicare covers emergency room visits for injuries, sudden illnesses or an illness that gets worse quickly. Medicare Advantage also provides emergency room coverage.
Medicare beneficiaries made between 4.2 and 5.3 million visits — depending on the definition — to an ER in 2012, according to an article in the journal Academic Emergency Medicine.
Medicare covers emergency room visits throughout the United States, but it typically doesn't cover emergency care outside the U.S., except in limited circumstances. Some Medigap policies cover foreign travel emergency care with a lifetime limit of $50,000. Some Medicare Advantage plans provide limited coverage for foreign travel emergencies.
Medicare Part A covers hospital or inpatient care. A person usually visits the ER at a hospital. However, there is a difference between emergency care at a hospital and being a hospital inpatient.
If Medicare Part B does pay some of the ER costs, you still pay: 1. A copayment for each ER visit. A copayment for each hospital service. 20% of the Medicare-approved amount for your doctor's services. The Part B deductible ($240 in 2024) Explore Humana Medicare Advantage plans.
With original Medicare, the coverage of emergency room and urgent care visits falls under Part B. The costs include a 20% coinsurance after paying the annual deductible of $203. If an emergency ...
Emergency room services are typically provided when you have a medical condition that requires immediate action, such as an injury or sudden illness. If you have a Medicare Advantage Plan, be aware that: Your plan cannot require you to see an in-network provider. You do not need a referral. There are limits on how much your plan can bill you if ...
Medicare covers emergency room visits when you get qualified care, such as medically necessary treatment for a sudden illness or injury. If your emergency room visit results in a doctor admitting you to the hospital as an inpatient within 3 days of your ER visit, Medicare Part A will cover your emergency room visit as well as your inpatient ...
It's important to note that while Medicare does cover emergency room visits, there are costs associated with these visits. Medicare Part B typically covers 80% of the Medicare-approved amount for emergency room services after you meet the yearly Part B deductible. However, if you're admitted to the hospital as an inpatient after being ...
Emergency room copayments and coinsurance. Even if your emergency room visit is covered by Medicare, you are typically responsible for paying a portion of the costs, known as copayments or coinsurance. Typically, you pay a Medicare emergency room copayment for the visit itself and a copayment for each hospital service.
Since Medicare Advantage plans are required to cover the same costs as Original Medicare, they also cover emergency room visits. The only difference between Advantage plans and Original Medicare is your out-of-pocket costs are different and less predictable. While Advantage plans provide more coverage them Medicare alone, they do not provide as ...
Original Medicare Original Medicare is a fee-for-service health insurance program available to Americans aged 65 and older and some individuals with disabilities. Original Medicare is provided by the federal government and is made up of two parts: Part A (hospital insurance) and Part B (medical insurance). will cover at least a portion of your visit to the emergency room.
Anyone with Part B will be covered for trips to a hospital emergency room. You will pay a copayment for the emergency department visit and a copayment for each hospital service. You also pay 20% of the Medicare-approved amount for your doctor's services and the Part B deductible applies. If you are admitted to the same hospital for a related ...
Medicare Advantage covers ER visits anywhere in the U.S., and you aren't required to use in-network hospitals for emergency care. However, each Medicare Advantage plan sets its own cost terms for ER visits. These costs can differ from Original Medicare. For example, a Medicare Advantage plan may require you to pay a copayment per visit that ...
Emergency Room Care a Priority For Older Adults . Emergency room visits are a medical necessity for many older adults. Falls are a leading cause of emergency room visits for older adults with Medicare in 2023, and other common reasons for emergency care include chest pain or stroke, car accidents, and heat-induced exhaustion. Medicare Part A and Part B, also called Original Medicare, works ...
Your hospital status—whether you're an inpatient or an outpatient—affects how much you pay for hospital services (like X-rays, drugs, and lab tests ). Your hospital status may also affect whether Medicare will cover care you get in a skilled nursing facility (SNF) following your hospital stay. You're an inpatient starting when you're ...
The ER is best equipped to see people with unexpected, intense and immediate symptoms or injuries, such as chest pain, difficulty breathing, or severe bleeding. But many other health problems can be addressed more quickly in other settings. In fact, as many as one in four ER visits could be handled at an urgent care center 1.
Medicare, trying to do a ... But while early research found the service, called Chronic Care Management, reduced emergency room and in-patient hospital visits and lowered total health spending, ...
Taylor said there's the traditional Medicare plan, which covers hospital visits and ER visits, but added those have a deductible. "You also can buy a plan called a Part D plan that covers your ...
Claims in the Outpatient and Inpatient files are identified via Revenue Center Code values of 0450-0459 (Emergency room) or 0981 (Professional fees-Emergency room). Claims in the MedPAR file are identified via the Emergency Room Charge Amount field when the amount is > $0. Although one can assume ER patients found in the inpatient data were ...
While boarding can happen to all ER patients, adults 65 and older, who account for nearly 20% of ER visits, are especially vulnerable during long waits for care. Also, seniors may encounter ...
But while early research found the service, called Chronic Care Management, reduced emergency room and in-patient hospital visits and lowered total health spending, uptake has been sluggish ...
This final rule will revise the Medicare Advantage (Part C), Medicare Prescription Drug Benefit (Part D), Medicare cost plan, and Programs of All-Inclusive Care for the Elderly (PACE) regulations to implement changes related to Star Ratings, marketing and communications, agent/broker compensation, health equity, dual eligible special needs ...
The Supreme Court considers whether Idaho's near-total abortion ban conflicts with a federal law aimed at ensuring certain standards for emergency medical care for patients, including pregnant women.